Understanding Fentanyl: The Risks & Navigating Recovery

What Makes Fentanyl Outpatient Treatment Maine Critical
Extreme Potency and Overdose Risk
For professionals and individuals navigating substance use, understanding the specific mechanics of fentanyl is essential for safe recovery planning. Fentanyl outpatient treatment Maine addresses a substance that presents a unique pharmacological challenge: it is approximately 50 to 100 times more potent than morphine. This extreme potency means that the margin between a therapeutic or euphoric dose and a lethal dose is microscopically small—often no larger than a few grains of salt.
When fentanyl enters the system, it binds rapidly to opioid receptors in the brain areas controlling pain and respiration. Unlike other opioids, the onset is immediate and the respiratory depression can be profound. If the dosage exceeds the body's tolerance, the brain ceases to send signals to the lungs, leading to hypoxia and death. This physiological reality drives the high mortality rates associated with the drug; in 2024, fentanyl was involved in 91% of opioid overdose deaths in specific regions.2
"Because of this high risk, fentanyl outpatient treatment Maine requires careful medical supervision, education about overdose prevention, and rapid access to life-saving tools like naloxone."
Effective treatment protocols must account for this volatility. Clinical supervision, rapid response capabilities, and education on physiological responses are foundational to the recovery process.
Contamination in the Drug Supply
A significant complication for those seeking recovery is the prevalence of contamination within the illicit drug supply. Many individuals who primarily use other substances—such as cocaine, methamphetamine, or counterfeit prescription pills—may unknowingly ingest fentanyl. This "lacing" creates a scenario where the user has no tolerance for the opioid, drastically increasing the likelihood of an adverse event.
Law enforcement data indicates a sophisticated manufacturing process where fentanyl is pressed into pills that mimic legitimate pharmaceuticals like Xanax or OxyContin. In 2024, authorities seized quantities of illicit fentanyl sufficient to cause hundreds of millions of fatalities, primarily disguised as other medications. This unpredictability necessitates a vigilant approach to treatment.1
Harm Reduction Strategies in Outpatient Care:
- Fentanyl Test Strips: Utilizing detection tools to identify the presence of opioids in other substances.
- Naloxone Distribution: Ensuring access to overdose reversal medication.
- Education: Understanding that contamination can occur in any illicitly purchased substance.
Coastal Recovery Partners emphasizes harm reduction as a core component of the intake and treatment process, ensuring that patients are equipped with the knowledge to navigate these risks safely.
Who Is Most Affected by Fentanyl
Demographic Patterns in Overdose Deaths
Analyzing demographic data reveals distinct patterns regarding who is most vulnerable to fentanyl-related adverse events. While addiction does not discriminate based on professional status or background, statistical trends highlight specific risk groups. Adults between the ages of 26 and 64 currently experience the highest rates of overdose deaths, with the 26-39 age cohort being particularly impacted. Furthermore, data indicates a gender disparity, with men dying from fentanyl overdoses at rates significantly higher than women in certain jurisdictions.2
Socioeconomic factors also play a critical role. High-stress environments, lack of stable housing, and barriers to healthcare access correlate with increased risk. Additionally, systemic health inequalities have resulted in disproportionately high overdose rates among Black and American Indian/Alaska Native populations. Understanding these demographics allows providers to tailor fentanyl outpatient treatment Maine programs to address the specific psychosocial stressors affecting these groups.9

The Emerging Xylazine Threat
The treatment landscape has been further complicated by the emergence of xylazine, a non-opioid veterinary sedative often referred to as "tranq." When combined with fentanyl, xylazine extends the duration of the sedative effect but introduces new medical risks that standard opioid protocols may not fully address.
Why Xylazine Complicates Overdose Response
Xylazine is not an opioid, meaning it does not respond to naloxone (Narcan). While naloxone should still be administered to reverse the fentanyl component of an overdose, it will not reverse the sedation caused by xylazine. This can lead to prolonged unconsciousness and requires specialized medical attention.
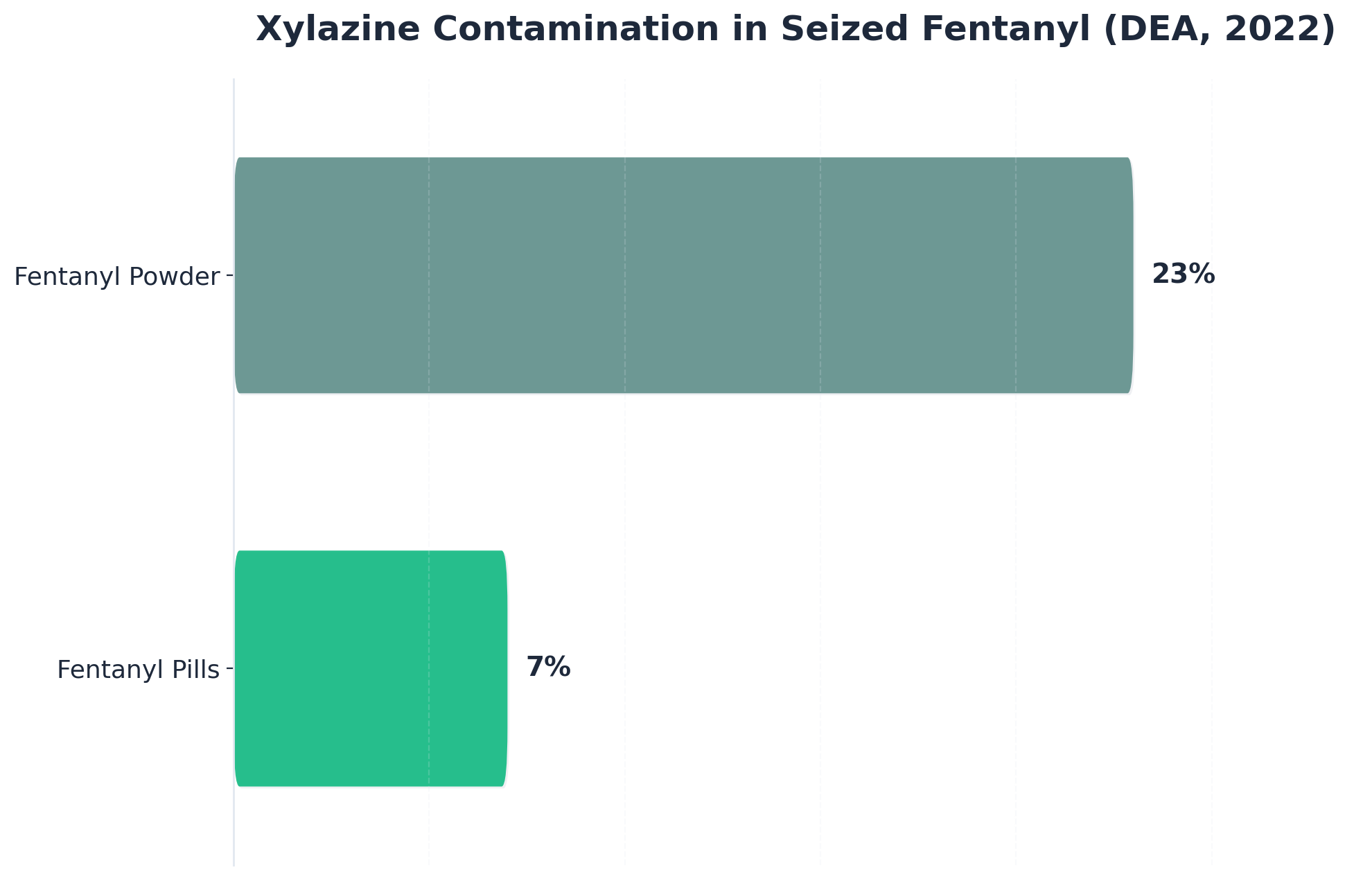
The Drug Enforcement Administration reported that in 2022, approximately 23% of seized fentanyl powder and 7% of pills contained xylazine. Beyond overdose risks, xylazine is associated with severe necrotic skin ulcerations that can occur regardless of the route of administration. For professionals in recovery, awareness of this contaminant is vital, as it necessitates specific wound care protocols and medical monitoring that are integral parts of comprehensive outpatient care.6
Evidence-Based Fentanyl Outpatient Treatment Maine Approaches
Medication-Assisted Treatment Outcomes
Medication-Assisted Treatment (MAT) serves as the clinical cornerstone for treating opioid use disorders. Rather than substituting one addiction for another, MAT utilizes FDA-approved medications—such as buprenorphine (Suboxone) and methadone—to normalize brain chemistry. These medications occupy opioid receptors to block the euphoric effects of fentanyl while simultaneously alleviating the debilitating physical withdrawal symptoms and cravings that often drive relapse.
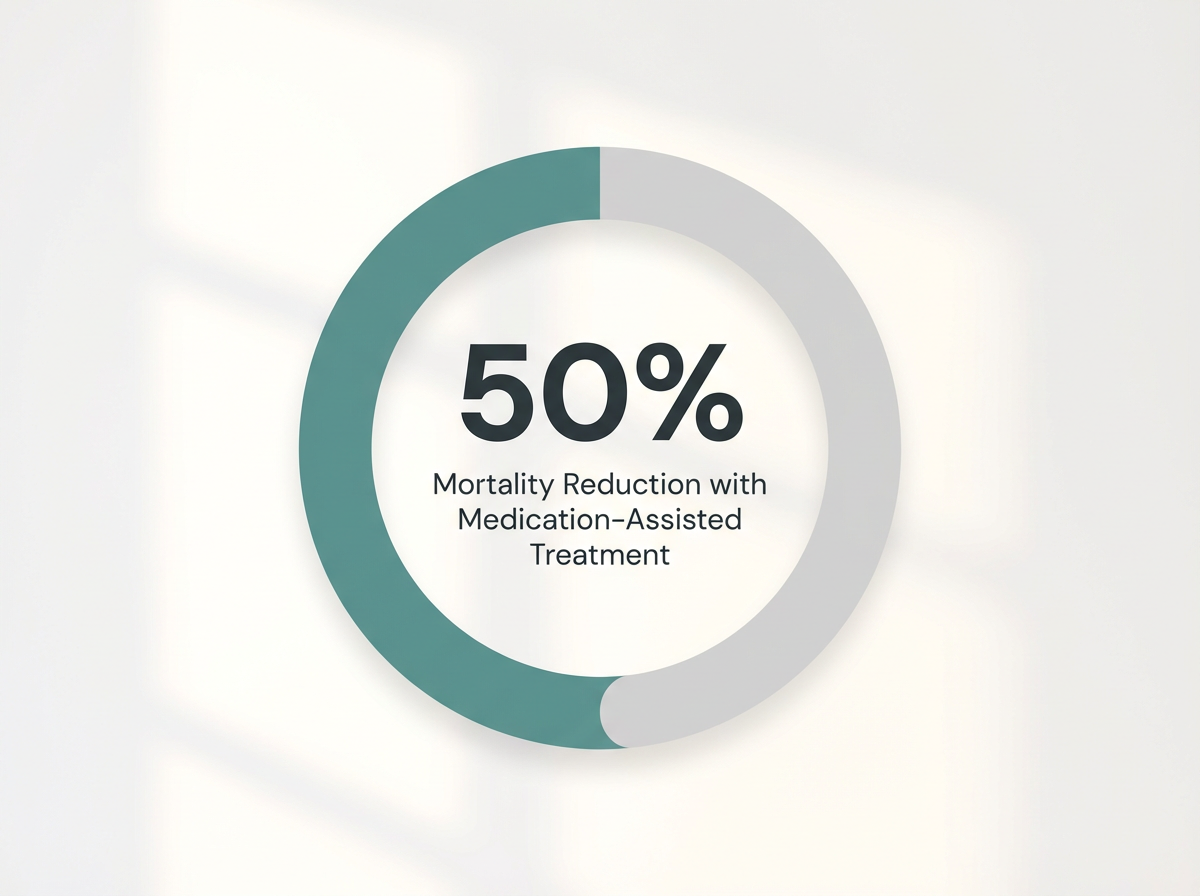
The efficacy of this approach is well-documented. Clinical studies indicate that MAT can reduce the mortality risk associated with opioid use disorder by approximately 50%. For working professionals, MAT provides the physiological stability required to engage fully in therapy and maintain employment. It functions as a stabilizing foundation, allowing the brain to heal and cognitive functions to return to baseline.7
At Coastal Recovery Partners, MAT is integrated into a broader recovery plan. Regular medical check-ins ensure dosages are optimized for the individual, minimizing side effects and maximizing stability. This medical management is not a crutch but a validated medical intervention for a chronic condition.
Integrated Behavioral Therapies
While medication addresses the physiological aspects of addiction, behavioral therapies address the psychological and behavioral patterns. Fentanyl outpatient treatment Maine employs evidence-based modalities to help individuals rewire cognitive pathways and develop resilience against triggers. Given that approximately 35% of adults with mental health disorders also struggle with substance use, integrated dual diagnosis care is essential.8
These therapies are delivered through both individual counseling and group sessions. Group settings offer peer support, allowing professionals to connect with others facing similar challenges, reducing isolation, and fostering a community of accountability.
Fentanyl Outpatient Treatment Maine for Working Adults
Balancing career responsibilities with recovery needs presents a significant challenge for working professionals seeking addiction treatment. Traditional residential programs often require extended time away from work, creating barriers that prevent many individuals from accessing the care they need. Outpatient treatment offers a practical alternative, providing comprehensive therapeutic support while allowing professionals to maintain their employment and daily commitments.
For many working professionals, the recovery journey begins with an Intensive Outpatient Program (IOP). This level of care delivers structured treatment through multiple weekly sessions, typically ranging from nine to twelve hours per week. The format provides substantial clinical support through evidence-based therapies including Cognitive Behavioral Therapy (CBT) and Dialectical Behavioral Therapy (DBT). Crucially, IOPs offer flexible scheduling—morning, afternoon, and evening options—allowing a financial analyst or executive to attend treatment without disrupting their workday.
When recovery needs are more complex or immediate, Partial Hospitalization Programs (PHP) serve individuals requiring more intensive support than IOP but who do not require 24-hour residential care. These programs typically involve:
- Five to six hours of treatment daily, five days per week.
- Comprehensive care coordination and medication management (MAT).
- Integrated dual diagnosis treatment for co-occurring mental health conditions.
This level of care proves particularly valuable for professionals transitioning from higher levels of care or managing complex recovery needs. Many individuals start with PHP to establish a strong foundation, then step down to IOP as they gain stability.
As recovery stabilizes, Standard Outpatient Programs (OP) provide ongoing support. With fewer weekly hours required, these programs focus on relapse prevention, coping skills training, and long-term recovery planning. This progression creates a continuum of care that adapts to changing needs rather than forcing individuals into a one-size-fits-all approach.
Coastal Recovery Partners structures its fentanyl outpatient treatment Maine programs specifically for working adults. The facility's flexible scheduling options, trauma-informed care model, and evidence-based therapeutic approaches create a treatment environment where professionals can address substance use disorders without sacrificing career stability. Care coordination services help navigate insurance coverage and treatment planning, removing administrative barriers that often delay access to care.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Frequently Asked Questions
Can someone recover from fentanyl addiction while maintaining their job and daily responsibilities?
Yes, recovery from fentanyl addiction is possible while maintaining a job and daily responsibilities. Outpatient programs are specifically designed to help working adults and professionals fit treatment into their schedules. These programs offer flexible options, including morning, afternoon, or evening sessions, so people can attend therapy and medical appointments around work or family needs. Medication-assisted treatment (MAT) and behavioral therapies are often included, making it easier to manage cravings and stress without missing important commitments. Research shows that combining MAT with outpatient care can reduce the risk of overdose death by about 50%. Fentanyl outpatient treatment Maine supports stability and helps individuals rebuild healthy routines.7
How long does medication-assisted treatment need to continue for optimal outcomes?
The length of medication-assisted treatment (MAT) for fentanyl addiction varies for each person. Research suggests that remaining on MAT for a year or longer leads to the best outcomes, as stopping too soon can raise the risk of relapse and overdose. Some people may need MAT for several years, much like someone with diabetes might need long-term insulin. Regular check-ins with a healthcare provider help decide when, or if, it is safe to taper off. Fentanyl outpatient treatment Maine uses ongoing assessment to keep treatment flexible and focused on lasting recovery.7
What should someone do if they suspect fentanyl contamination in substances they or someone they know has used?
If fentanyl contamination is suspected in any substance, the safest step is to avoid using it and encourage others to do the same. Fentanyl is so strong that even a tiny, hidden amount can cause a life-threatening overdose. Anyone who has already used a possibly contaminated substance should not use alone, and someone nearby should have naloxone ready, as it can reverse an opioid overdose even though it may not work against all possible additives like xylazine. Fentanyl outpatient treatment Maine programs recommend using test strips to check for fentanyl and seeking medical advice right away if overdose symptoms appear, such as very slow breathing or unresponsiveness.6
Is fentanyl addiction different from other opioid addictions in terms of treatment approach?
Yes, fentanyl addiction is different from other opioid addictions in terms of treatment approach. Fentanyl’s extreme potency means withdrawal can start faster, feel more intense, and sometimes last longer than with drugs like heroin or prescription painkillers. This makes careful medical supervision even more important. Outpatient programs in Maine often use higher doses or longer courses of medication-assisted treatment and focus on overdose education because the risk is so high. Treatment teams may also add extra support for managing cravings and preventing relapse. These differences help fentanyl outpatient treatment Maine provide safer, more effective care for people facing this unique challenge.7
How does co-occurring mental health treatment integrate with fentanyl addiction recovery?
Co-occurring mental health treatment is closely integrated with fentanyl addiction recovery because many people face both challenges at once. In fact, about 35% of adults with a mental health disorder also have a substance use disorder, so treating only one issue often leads to setbacks. Integrated care means therapy and medical support are provided together, not separately. For example, someone dealing with anxiety and fentanyl use will get therapy for both—like learning coping skills for anxiety while also managing cravings. Fentanyl outpatient treatment Maine programs often use this approach so professionals can address root causes, reduce relapse risk, and support overall well-being.8
What role does insurance play in accessing comprehensive fentanyl treatment programs?
Insurance plays a crucial role in making fentanyl outpatient treatment Maine accessible for working professionals and their families. Most comprehensive insurance plans help cover key services, including medication-assisted treatment, behavioral therapies, and care for co-occurring mental health conditions. This support allows more people to receive coordinated care without overwhelming out-of-pocket costs or disrupting work schedules. Think of insurance as a bridge—it helps connect individuals to the right mix of medical and counseling services needed for long-term recovery. National guidelines highlight the importance of insurance and financial access in improving treatment rates and outcomes for opioid use disorder.4
Conclusion
For professionals navigating the decision to seek treatment, the central question often isn't whether recovery is necessary—it's whether it's feasible. The reality is that outpatient care is specifically designed to integrate with existing commitments rather than replace them. By offering structured therapeutic support during hours that accommodate work schedules, these programs acknowledge that recovery happens within the context of real life, not separate from it.
The combination of evidence-based therapies, trauma-informed approaches, and medication-assisted treatment creates a clinical framework that addresses both immediate symptoms and underlying factors. This isn't about quick fixes or temporary abstinence—it's about building sustainable skills for managing triggers, processing difficult emotions, and maintaining sobriety while continuing to meet professional and personal obligations. The flexibility of Intensive Outpatient, Partial Hospitalization, and standard Outpatient programs means treatment intensity can match current needs without requiring a complete life pause.
For those in the South Portland area, Coastal Recovery Partners offers morning, afternoon, and evening treatment options alongside dual diagnosis and MAT services. The path forward involves assessing which level of care aligns with current circumstances, understanding what insurance will cover, and recognizing that seeking support is a professional decision—one that protects both career and well-being. Recovery doesn't demand perfection or isolation; it requires showing up consistently and allowing the process to work alongside the life that's already been built.
Remember that recovery is a journey of rebuilding trust—in yourself, in others, and in the process of healing. If you are ready to explore your options, reach out to Coastal Recovery today. We're here to help guide you toward a future defined not by your past, but by your resilience and hope.
References
- Psychiatry.org - Opioid Use Disorder. https://www.psychiatry.org/patients-families/opioid-use-disorder
- Los Angeles County Department of Public Health - Fentanyl-Overdoses-in-Los-Angeles-County.pdf. http://lapublichealth.org/sapc/MDU/SpecialReport/Fentanyl-Overdoses-in-Los-Angeles-County.pdf
- World Health Organization - Opioid Overdose. https://www.who.int/news-room/fact-sheets/detail/opioid-overdose
- SAMHSA - Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov
- CDC - Drug Overdose Deaths in the United States, 2023-2024. https://www.cdc.gov/nchs/products/databriefs/db549.htm
- DEA - Reports Widespread Threat of Fentanyl Mixed with Xylazine. https://www.dea.gov/alert/dea-reports-widespread-threat-fentanyl-mixed-xylazine
- NCBI - The Effectiveness of Medication-Based Treatment for Opioid Use Disorders. https://www.ncbi.nlm.nih.gov/books/NBK541393/
- NIDA - Co-Occurring Disorders and Health Conditions. https://nida.nih.gov/research-topics/co-occurring-disorders-health-conditions
- KFF - Opioid Overdose Deaths: National Trends and Variation by Demographics and States. https://www.kff.org/mental-health/opioid-overdose-deaths-national-trends-and-variation-by-demographics-and-states/
- Congress.gov - Illicit Fentanyl and Mexico's Role. https://www.congress.gov/crs-product/IF10400





