Understanding Trauma Focused Cognitive Behavioral Therapy

Key Takeaways
- TF-CBT moves through eight paced PRACTICE phases, building psychoeducation, relaxation, and coping skills before the trauma narrative is ever spoken aloud 8, 11.
- You don't need to be sober first — integrated care treats PTSD and substance use together, and shifts in PTSD often drive reductions in substance use 1, 4.
- Evidence shows large within-group reductions in post-traumatic stress symptoms (g = 1.14) and meaningful gains in dual diagnosis care, with stronger effects on trauma than substance use 13, 15.
- Outpatient IOP, PHP, and standard tracks let TF-CBT run alongside MAT and dual diagnosis support, with aftercare protecting gains that can fade by eight months 5, 6.
"Will I Have to Relive It?" The Question That Keeps People Out of Trauma Therapy
That's the question, isn't it? The one that sits in your throat when someone says the word trauma therapy. Will I have to tell the whole story? Out loud? In detail? On a Tuesday afternoon, with a stranger, in a quiet room?
If your chest tightens at the thought, that makes sense. You've spent a long time keeping certain memories at arm's length. Maybe a drink helped. Maybe a pill. Maybe just staying so busy you never had to sit still long enough to feel it. And now someone is suggesting you walk straight toward the thing you've been outrunning.
Here's what most people aren't told up front: trauma-focused cognitive behavioral therapy, or TF-CBT, is not one big confession session. It's not a movie scene where you break down on a couch and relive the worst day of your life. It's a paced, structured approach that spends real time teaching your nervous system how to feel safe before it ever asks you to talk about what happened 8, 11.
And if substances have been part of how you've coped, you're not disqualified. You don't have to be perfectly sober to begin. The research on co-occurring PTSD and substance use is clear that people can tolerate and benefit from this work while addiction care is still happening 1.
So take a breath. Showing up to read this counts. Let's walk through what TF-CBT actually is, gently, one piece at a time.
What TF-CBT Actually Is (In Plain Language)
A Phased, Paced Approach — Not One Big Confession Session
Picture it less like jumping off a cliff and more like wading into the ocean off Willard Beach. You stand on the sand first. Then you let the water touch your ankles. Then your knees. You don't get pushed in.
TF-CBT is built that way on purpose. It's a structured therapy with eight distinct phases, and the trauma story itself doesn't show up until well into the process. Before you ever talk about what happened, your therapist spends real, unhurried time helping you understand how trauma affects your brain and body, and teaching you specific skills to calm your nervous system when memories surface 8, 11.
That pacing matters, especially if substances have been part of how you've gotten through hard nights. The model was designed knowing that people sometimes use avoidance — including substance use — to push memories down, and that pushing them down can actually make symptoms worse over time 7. So instead of asking you to white-knuckle through, TF-CBT gives you better tools first.
You will not be ambushed. You will not be asked to perform your worst day for a stranger. The pace is collaborative, and you have a say in it the whole way through.
The PRACTICE Framework, Translated
TF-CBT clinicians use a memory aid called PRACTICE to organize the eight phases. Each letter stands for a piece of the work. Here's what each one actually feels like, in plain language.
P — Psychoeducation. You learn what trauma does to a brain and body. Why you flinch at certain smells. Why your sleep is wrecked. Why a craving can hit out of nowhere. This part alone can be a relief: you're not broken or weak, you're having a recognizable response.
R — Relaxation. Concrete skills for the body — slow breathing, grounding, simple exercises you can do in your car before a shift. This is the part that gives you something to do when the panic rises.
A — Affective regulation. A clinical phrase for a simple idea: learning to name what you're feeling and ride it out without numbing it. Anger, shame, grief, all of it.
C — Cognitive coping. Catching the thoughts that keep the pain looping. The "it was my fault" thought. The "I'm too damaged" thought. You learn to spot them and try on truer ones.
T — Trauma narrative. Yes, this is the part you've been bracing for. And by the time you get here, you've already built the skills to do it without falling apart. It's gradual, written or spoken in pieces, on your timeline.
I — In vivo mastery. Slowly facing safe reminders you've been avoiding — a road, a grocery store, a song — so they stop running your life.
C — Conjoint sessions. Bringing in a trusted support person, when that's helpful and safe, so the people around you understand what you're doing.
E — Enhancing safety. Practical planning for the future: relapse prevention, safety skills, what to do when something hard happens next month or next year.
That whole arc is what gives TF-CBT its evidence-based standing with bodies like SAMHSA 11, and it's why the structure itself — skills first, story later — is part of why it works 8.
Why Trauma and Substance Use Belong in the Same Room
The Myth That You Have to Be Sober First
You've probably heard some version of this: "Get clean first, then we'll deal with the trauma." Maybe a counselor said it. Maybe a family member. Maybe it was the voice in your own head, the one that says you haven't earned the right to look at the hard stuff yet.
That advice sounds protective. It isn't. For a lot of people, the trauma is exactly what's driving the substance use, and being told to white-knuckle through sobriety without addressing the reason you started numbing in the first place is like being told to stop bailing water without anyone fixing the hole in the boat.
There's also a quieter reason this myth hangs on. Pushing memories down — through substances, through avoidance, through staying constantly busy — can actually make trauma symptoms worse over time, not better 7. Waiting until you're "ready" can mean waiting forever. Showing up imperfect, still wobbling, is allowed. That's the whole point.
Treating PTSD Is What Moves the Substance Use
Here's the part that surprises people: in integrated care, when the trauma piece starts to shift, the substance use often starts to shift with it. Not the other way around.
A 2025 study looked at exactly this question — what's actually doing the work in integrated treatment for people with both PTSD and a substance use disorder? The finding was telling. Changes in PTSD severity were a key driver of improvement in substance use symptoms 4. Translation: when the nightmares ease up, when the hypervigilance settles, when the shame loosens its grip, the pull toward the bottle or the pill quiets down too. The trauma was doing more of the steering than people realized.
That changes what "good care" looks like. The old sequential model — finish addiction treatment, then maybe years later try trauma therapy — leaves the engine of the problem running. Integrated care addresses both at once, in the same room, with clinicians who understand how they feed each other 1.
This is the practical case for trauma-informed outpatient programs that fold TF-CBT into IOP, PHP, or standard outpatient care alongside MAT and dual diagnosis support. You're not getting two disconnected treatments stitched together. You're getting one coordinated plan that treats you as one person.
None of this is a guarantee. Integrated trauma-focused care tends to show stronger effects on PTSD than on substance use, and progress is uneven for everyone 15. But the direction is clear: leaving the trauma untreated is what keeps the substance use stuck. Addressing it — gently, in phases, with skills first — is what gives recovery something solid to stand on.
What TF-CBT Actually Changes Inside You
Here's something worth knowing: trauma isn't just a memory you carry. It's a memory that's stored differently — fragmented, raw, often without words, sometimes more like a smell or a feeling in your stomach than a story with a beginning and end. That's why a song on the radio can drop you to your knees ten years later. The memory hasn't been filed properly. It's still loose in the system.
What TF-CBT does, slowly, is help your brain refile it.
A 2025 study looking at adolescents with complex PTSD found that TF-CBT produced real, measurable shifts in three areas that survivors will recognize:
- the quality of the trauma memory itself,
- dissociation (those moments when you check out, go numb, or lose time), and
- body image — that uneasy, sometimes hateful relationship with your own skin that trauma so often leaves behind 3.
The memory becomes more coherent. The dissociation eases. The body starts to feel like home again instead of a crime scene.
You may notice it in small ways at first. A trigger that used to wreck your whole afternoon only takes an hour. You can sit through a meal without drifting out. You catch yourself in the mirror and don't immediately look away.
Those shifts matter for recovery in a particular way. When the memory loses its raw electrical charge, the urge to numb it loses some of its force too. You're not white-knuckling against a feeling that won't quit — the feeling itself is changing shape 4. That's the inside work. That's what you can't see from the outside but absolutely feel from within.
Does It Actually Work? An Honest Look at the Evidence
You deserve a straight answer here, not a sales pitch. So here's what the research actually says — the strong parts and the parts that are still being figured out.
The biggest meta-analysis to date pulled together 28 randomized controlled trials and 33 uncontrolled studies on TF-CBT for people exposed to physical and sexual intimate partner violence. Within-group improvement on post-traumatic stress symptoms was large — a Hedges' g of 1.14 (CI 0.97–1.30). Compared to control groups, TF-CBT still came out ahead with a moderate-to-large effect of g = 0.52 (CI 0.31–0.73) 13. In plain English: people who did TF-CBT got significantly better, and they got better faster than people who didn't.
One important caveat, because you should know it: that meta-analysis drew heavily from youth and intimate partner violence samples. The numbers are real, but they don't perfectly map onto every adult walking into outpatient care with a long history of substance use. Take the direction seriously; hold the exact size loosely.
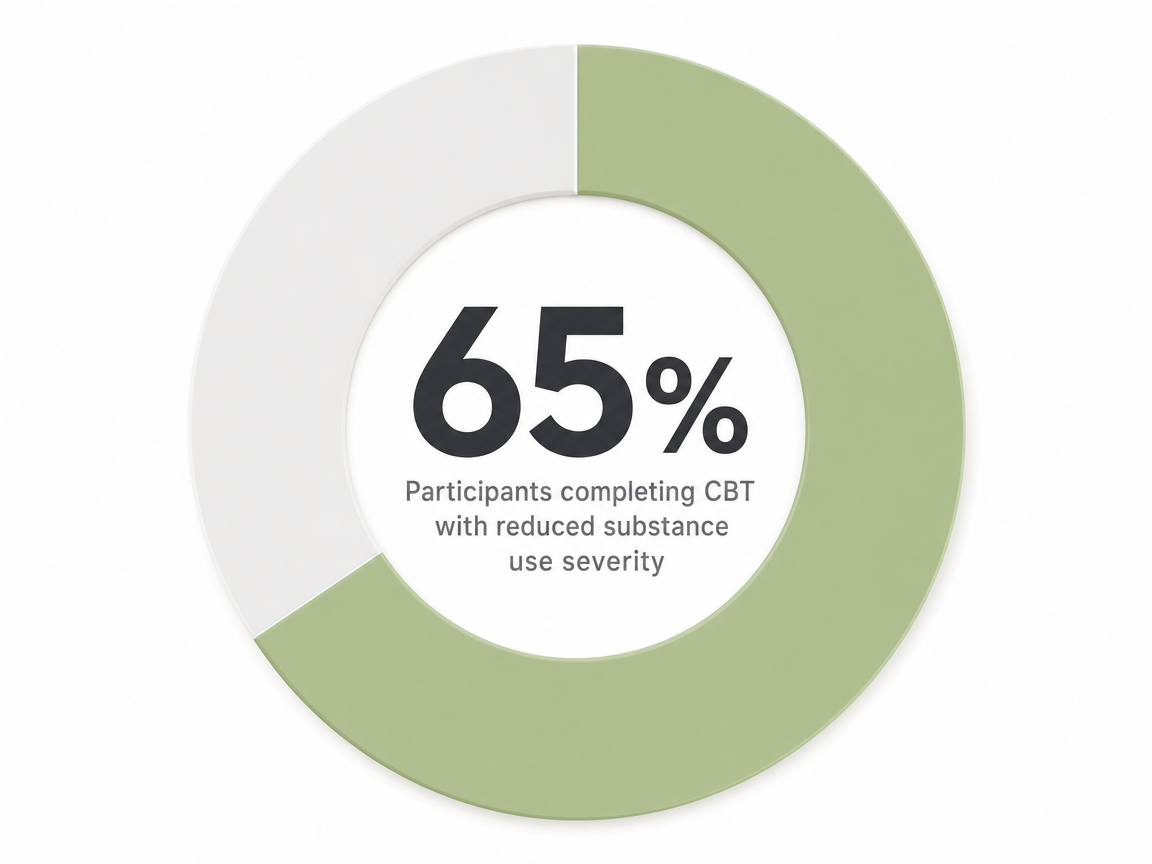
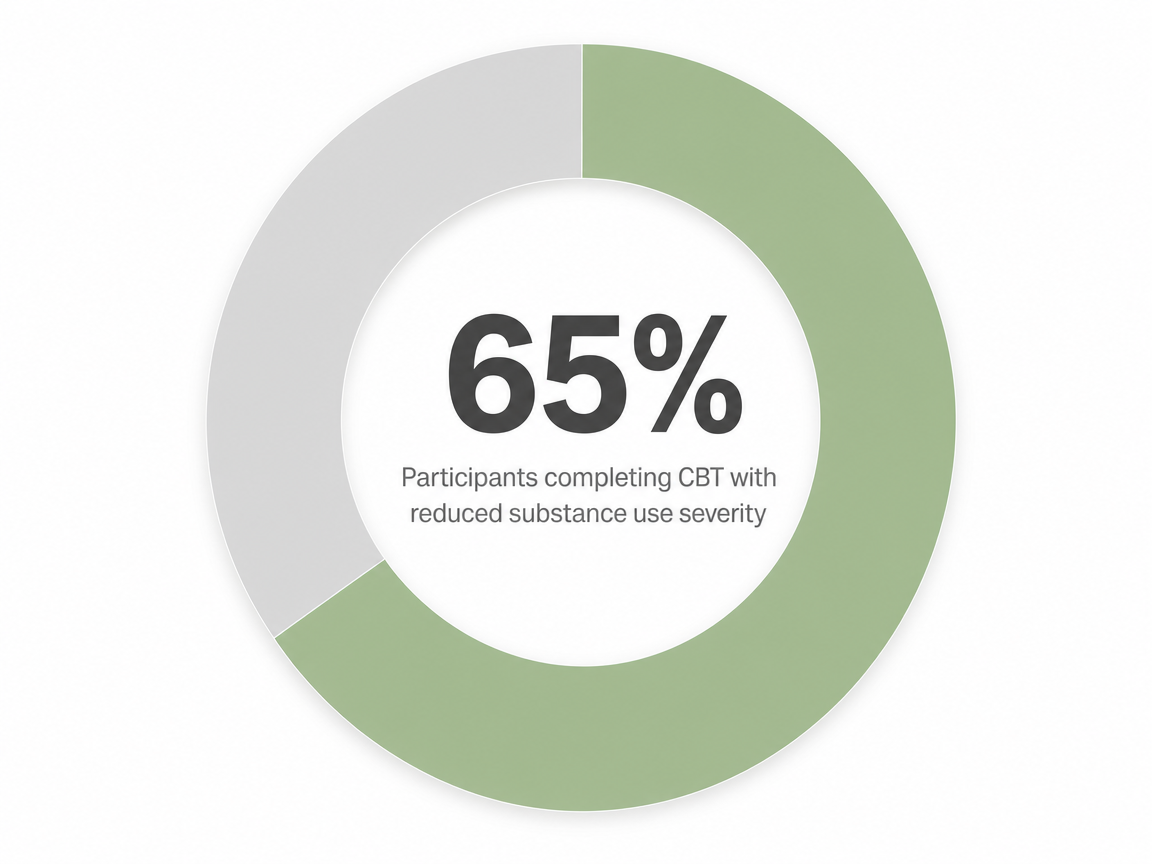
For dual diagnosis specifically, the picture is more modest but still encouraging. A trial of CBT designed for co-occurring PTSD and substance use disorder saw 65% of participants complete therapy and meaningful reductions in substance use severity 14. The VA's review of integrated trauma-focused care found it superior to alternatives, with stronger effects on PTSD than on substance use — honest, not flashy 15. A 2025 review of CBT for dual diagnosis reached a similar verdict: real improvement in mental health and substance use symptoms, with results that vary person to person 10.
And the broader CBT-for-substance-use literature shows small to moderate effects compared to inactive controls, with some fade by the eight-month mark 6. That's not a knock on the therapy — it's a case for aftercare, alumni support, and not treating the end of a structured program as the end of the work.
So does it work? Yes — meaningfully, measurably, and especially for trauma symptoms. Is it a magic eraser? No. What you can reasonably expect is a real shift in how the trauma sits inside you, less pull toward numbing, and a foundation strong enough to keep building on.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
How TF-CBT Fits Into Outpatient Care, MAT, and Dual Diagnosis Support
So how does this actually look on a regular Wednesday, when you also have a job, a kid to pick up from school, and maybe a Suboxone dose to take in the morning?

This is where outpatient programs earn their keep. TF-CBT was built to be delivered in structured, recurring sessions — exactly the rhythm that an Intensive Outpatient Program (IOP), Partial Hospitalization Program (PHP), or standard outpatient track is designed to provide. You go to treatment several times a week, do the work, and come home. You sleep in your own bed. You keep your job. The eight phases of TF-CBT unfold over weeks, alongside the rest of your recovery plan, instead of being squeezed into a single residential stay.
If you're on medication-assisted treatment, this matters even more. Medications like buprenorphine or naltrexone do something important — they quiet the loudest parts of the addiction so you have the bandwidth to do the deeper work. A study of patients with co-occurring PTSD and opioid use disorder found that those receiving MAT plus integrated CBT had significantly decreased odds of a positive urine drug screen compared to MAT alone 5. The medication holds the floor steady; the therapy rebuilds the room.
Dual diagnosis support is the third leg of the stool. If you're carrying PTSD plus depression, anxiety, or another co-occurring condition, a dual diagnosis team treats those together rather than ping-ponging you between providers who don't talk to each other. A 2025 review of CBT-based care for dual diagnosis found real improvement in both mental health and substance use symptoms when interventions were delivered in coordinated outpatient settings 10.
What this looks like in practice: a trauma-informed clinician guiding you through the PRACTICE phases, a prescriber managing your MAT, a counselor helping with relapse prevention skills, and group sessions where you're not the only one in the room who knows what a 3 a.m. craving feels like. It's one team, one plan, scheduled around your real life — morning, afternoon, or evening — so you don't have to choose between getting better and keeping the lights on.
That coordination is the quiet engine behind everything else in this article. Without it, trauma work can feel destabilizing. With it, you have a container strong enough to hold the hard parts.
What to Expect in the First Few Weeks
The first few weeks of TF-CBT are quieter than most people expect. You will not walk into session one and be asked to start from the beginning. You'll probably talk about your week. Your sleep. How the cravings have been. What's been happening at home.
Then your therapist will start teaching.
Early sessions focus on the first letters of PRACTICE — psychoeducation, relaxation, and the beginnings of affective regulation 8, 11. You'll learn what your nervous system is actually doing when it floods. You'll practice a grounding skill in the room and try it again that night when you can't sleep. You might leave the first session with one small homework piece: notice when your shoulders climb up to your ears, and try the breathing thing. That's it.
Some weeks will feel productive. Some will feel slow. A few might leave you tired in a way you can't explain — that's the body unclenching after years of holding on. Going easy on yourself those nights is part of the work, not a detour from it.
If you're also in an IOP or PHP track, your TF-CBT sessions sit alongside group therapy, relapse prevention, and any MAT appointments you have. Your team talks to each other. If something gets stirred up in a trauma session on Tuesday, your group counselor on Wednesday already knows to check in.
Showing up to the second week counts. So does the third. The pace is the point.
Small Wins, Long Game: After the Trauma Narrative
Once you've made it through the trauma narrative — the part you spent weeks bracing for — something shifts. Not all at once. In small, almost unremarkable ways.
You hear the song that used to gut you and notice you're still standing in the kitchen, still chopping onions. A coworker says something that would have sent you to the parking lot for a smoke break, and you stay in the meeting. You sleep through the night. You sleep through two nights in a row. You realize, on a Thursday, that you haven't thought about the thing all day.
Those are the wins. Count them.
The later phases of TF-CBT — in vivo work, conjoint sessions if they fit, and enhancing safety — are where you take what you've built and bring it into your real life 8, 11. This is also where aftercare and alumni support earn their place. CBT for substance use shows real effects, but those effects can fade by the eight-month mark without ongoing support 6. The work doesn't end when the structured program does. It just changes shape — group check-ins, alumni meetings, a standing therapy slot when you need one. Long game, small wins, both at once.
A Quiet Note from the Coast
If you've read this far, something in you is already moving toward the work. That counts.
Trauma therapy isn't a single brave leap. It's a slow walk down to the water with someone who knows the tide. You'll learn what your nervous system is doing. You'll learn how to settle it. And only then, on your timeline, will you start to look at the parts of your story that have been waiting for you.
Outpatient care here in South Portland is built around real lives — work shifts, custody schedules, MAT appointments, the long Maine winter. If you're ready to talk to someone, the team at Coastal Recovery Partners can help you figure out what level of care fits.
You don't have to be ready. You just have to make the call.
Frequently Asked Questions
Do I have to be sober before I can start TF-CBT?
No. The Department of Veterans Affairs is direct that people with co-occurring PTSD and substance use disorder can tolerate and benefit from trauma-focused treatment, and one diagnosis should not block care for the other 1. If trauma is part of why you use, waiting to be perfectly sober first often keeps you stuck. You can begin imperfect.
Will TF-CBT make me relive my trauma in detail?
Not in the way you're picturing. TF-CBT is phased — you spend real time on psychoeducation, relaxation, and coping skills before the trauma narrative ever comes up 8, 11. When you do tell the story, it happens gradually, in pieces, on your timeline, with the skills already built. You won't be ambushed or pushed past what you can handle.
Can I do TF-CBT while I'm on MAT (medication-assisted treatment)?
Yes, and the combination tends to help. A study of patients with co-occurring PTSD and opioid use disorder found that those receiving MAT plus integrated CBT had significantly decreased odds of a positive urine drug screen compared to MAT alone 5. The medication steadies the ground; the therapy does the deeper work. They're designed to support each other, not compete.
How long does TF-CBT usually take?
The structured model unfolds across the eight PRACTICE phases, typically over several months of weekly or twice-weekly sessions 8, 11. In an outpatient program, it sits alongside group therapy, relapse prevention, and any MAT appointments you have. The pace depends on what you bring in, what's stirring up, and how much support you need each week. Slower can be better.
Does TF-CBT work if I've been through more than one trauma?
Yes. One of the persistent myths is that TF-CBT only fits a single, clean-edged event — but the evidence shows it helps people with complex profiles, including multiple traumas and ongoing substance use 7, 2. A 2025 study even found measurable improvements in trauma memory quality, dissociation, and body image among people with complex PTSD 3. You're not too complicated for this.
Can I keep working and parenting while doing this kind of therapy?
Yes — that's exactly what outpatient programs are built for. IOP, PHP, and standard outpatient tracks offer morning, afternoon, and evening sessions so treatment fits around shift work, custody schedules, and the rest of real life. You sleep at home, keep your job, pick up your kids. The work is real, but it's designed to happen alongside your life, not instead of it.
References
- Treatment of Co-Occurring PTSD and Substance Use Disorder in VA. https://www.ptsd.va.gov/professional/treat/cooccurring/tx_sud_va.asp
- Co-occurring trauma- and stressor-related and substance use disorders in youth: a narrative review. https://pmc.ncbi.nlm.nih.gov/articles/PMC11600332/
- Effectiveness of trauma-focused cognitive behavioral therapy delivered in individual and group settings on trauma-related memory quality. https://pmc.ncbi.nlm.nih.gov/articles/PMC12822885/
- How changes in post‐traumatic stress disorder (PTSD) severity mediate effects of integrated treatment on substance use disorder symptoms. https://pmc.ncbi.nlm.nih.gov/articles/PMC12529247/
- The Impact of Addiction Medications on Treatment Outcomes for Patients with Co-Occurring PTSD and Opioid Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC4866634/
- An Evaluation of Cognitive Behavioral Therapy for Substance Use Disorder: A Scoping Review of the Empirical Literature. https://pmc.ncbi.nlm.nih.gov/articles/PMC10572095/
- Ten misconceptions about trauma-focused CBT for PTSD. https://pmc.ncbi.nlm.nih.gov/articles/PMC7613703/
- Trauma-Focused Cognitive Behavioral Therapy. https://pmc.ncbi.nlm.nih.gov/articles/PMC4396183/
- Trauma-focused treatment for posttraumatic stress disorder (PTSD) and functional impairment following child abuse. https://pmc.ncbi.nlm.nih.gov/articles/PMC3698199/
- Cognitive Behavioural Therapy and Dual Diagnosis. https://pmc.ncbi.nlm.nih.gov/articles/PMC12535280/
- Trauma-Focused Cognitive Behavioral Therapy (TF-CBT) - SAMHSA. https://www.samhsa.gov/resource/dbhis/trauma-focused-cognitive-behavioral-therapy-tf-cbt
- A Randomized Implementation Study of Trauma-Focused Cognitive Behavioral Therapy in Residential Treatment Facilities. https://pmc.ncbi.nlm.nih.gov/articles/PMC5175405/
- A systematic review and meta-analysis of trauma-focused cognitive behavioral therapy for physical and sexual intimate partner violence. https://pubmed.ncbi.nlm.nih.gov/36155943/
- A cognitive behavioral therapy for co-occurring substance use and posttraumatic stress disorder. https://pmc.ncbi.nlm.nih.gov/articles/PMC2720425/
- Treatment for Co-Occurring Posttraumatic Stress Disorder and Substance Use Disorders. https://www.ptsd.va.gov/professional/articles/article-pdf/id1655729.pdf




