7 Examples of Trauma-Informed Care That Build Trust

Why These Examples of Trauma Informed Care Transform Recovery Outcomes
Implementing practical examples of trauma informed care fundamentally reshapes recovery by addressing the underlying experiences that often drive addiction. As treatment professionals, you recognize that research consistently shows individuals with trauma histories achieve significantly better outcomes when clinical protocols acknowledge this connection.1
Traditional approaches that overlook trauma can inadvertently trigger stress responses, undermining therapeutic progress and increasing dropout rates. When treatment teams understand how trauma affects the nervous system, emotional regulation, and coping mechanisms, they create environments where true healing becomes possible.2
"Safety-centered frameworks improve engagement rates, strengthen therapeutic relationships, and reduce crisis incidents during treatment."
This approach recognizes that many behaviors labeled as resistance or non-compliance are actually adaptive survival responses. By reframing these patterns, clinicians help individuals develop new skills without shame or judgment. Programs like Coastal Recovery Partners integrate these principles throughout their continuum, from Intensive Outpatient Programs (IOP) and Partial Hospitalization Programs (PHP) to standard Outpatient (OP) services.
This consistency ensures that whether a client attends morning, afternoon, or evening sessions, they experience the same safety-focused approach. Combined with proven therapies like Cognitive Behavioral Therapy (CBT), Dialectical Behavioral Therapy (DBT), and grounding skills, this trauma-sensitive foundation creates an environment where dual diagnosis treatment addresses both addiction and underlying mental health conditions effectively.

Building Trust Through Comprehensive Examples of Trauma Informed Care
Trust forms the foundation of effective treatment that honors past wounds, particularly when individuals have experienced systems that dismissed their pain or misunderstood the connection between early adversity and current dependency patterns. Comprehensive care addresses both conditions simultaneously as interconnected elements instead of treating them as separate issues requiring sequential attention.3
Integrated dual diagnosis treatment recognizes that psychological injury symptoms and dependency patterns reinforce each other, requiring coordinated intervention strategies. When treatment professionals understand how past adversity shapes coping mechanisms, they can design approaches that validate experiences while building healthier regulation skills.
Care ApproachClinical FocusExpected Business & Clinical OutcomeTraditional Sequential CareTreating addiction first, then traumaHigher attrition, lower trustIntegrated Trauma-Informed CareSimultaneous dual diagnosis treatmentImproved retention, stronger therapeutic alliance
This integration extends through all therapeutic modalities, from CBT and DBT to medication-assisted protocols that account for trauma-related medication sensitivities. Coastal Recovery Partners structures its day programs, hospital-level day treatment, and flexible outpatient services around this comprehensive model.
By combining research-supported therapies with explicit protocols that honor psychological wounds, treatment addresses root causes while moving beyond surface behaviors. Care coordination ensures consistency across all service touchpoints, creating the predictable, safe environment essential for healing. When individuals experience this level of integrated support, they can focus on recovery without navigating fragmented systems.
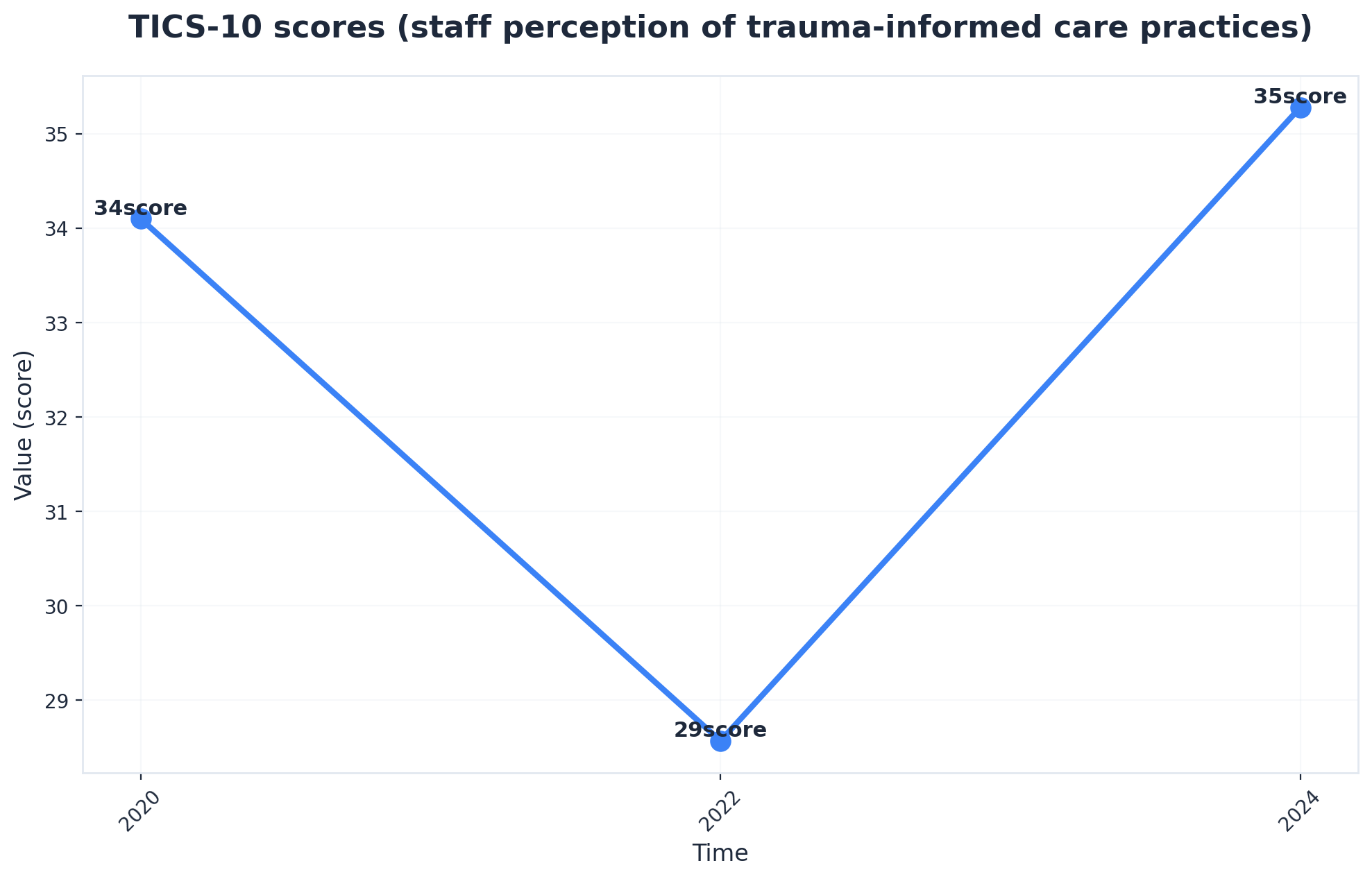
1. Universal Trauma Screening at Intake
Universal trauma screening at intake represents a foundational shift in how treatment programs identify and respond to the complex needs of individuals entering recovery. Instead of waiting for trauma histories to surface organically, comprehensive screening tools administered during the initial assessment create a baseline understanding of each person's experiences and potential triggers.4
Effective screening goes beyond simple yes-or-no questions. Validated instruments like the PTSD Checklist (PCL-5) or the Adverse Childhood Experiences (ACE) questionnaire provide clinicians with nuanced information about trauma types, severity, and current symptom presentation. For more detailed guidelines, professionals can refer to the SAMHSA Guidance for a Trauma-Informed Approach.
The screening process itself must embody trauma-informed principles. Clinicians conducting assessments should explain the purpose clearly, emphasize that participation is voluntary, and create space for individuals to decline specific questions without jeopardizing admission.
- Ensure Privacy: Conduct screenings in private, acoustically sound settings.
- Allow Adequate Time: Avoid rushing the intake process to prevent heightened anxiety.
- Train Staff: Ensure intake coordinators can recognize signs of distress or dissociation.
Programs offering structured outpatient and day treatment services benefit particularly from early trauma identification. Understanding trauma responses helps treatment staff anticipate challenges with attendance, emotional regulation during sessions, and interpersonal dynamics in group settings. This proactive approach prevents misinterpretation of trauma symptoms as resistance, ensuring individuals receive appropriate support from day one.
2. Choice-Centered Treatment Planning
Choice-centered treatment planning represents a fundamental shift from traditional directive approaches to collaborative care models. When individuals enter treatment with histories of trauma, they often carry experiences of powerlessness and loss of control. Recovery becomes more effective when treatment plans restore autonomy through meaningful participation in decision-making processes.5
Care providers can implement choice-centered planning by presenting multiple research-supported options instead of prescribing singular pathways. This might involve offering selections between group therapy modalities, individual session frequencies, or therapeutic approaches that align with personal learning styles. The American Psychological Association emphasizes that restoring agency is a critical component of trauma recovery.
Example of Choice-Centered Dialogue
Instead of saying, "You will attend CBT groups on Tuesdays," a clinician might say, "We have CBT groups on Tuesdays and DBT skills groups on Thursdays. Based on your goal of managing anxiety, which approach feels like a better starting point for you?"
Programs like IOP and PHP naturally support choice-centered planning through flexible structures. Treatment providers can work collaboratively to determine session timing, therapeutic modalities, and complementary supports such as medication-assisted approaches. This collaborative approach extends to dual diagnosis care, where individuals help shape how mental health and addiction treatment integrate within their recovery plan.
The practical benefits extend beyond engagement. When people actively participate in treatment design, they develop critical skills in self-advocacy and decision-making that transfer directly to long-term recovery. Documentation of these collaborative decisions becomes equally important, creating transparency that reinforces trust throughout the recovery journey.

3. Physical Environment Modifications
The physical treatment space itself communicates safety or threat before a single word is spoken. Survivors in recovery recognize how environmental triggers—harsh lighting, locked doors without explanation, institutional color schemes—can activate hypervigilance and undermine therapeutic engagement. Thoughtful facility design acknowledges this reality by creating spaces that support nervous system regulation instead of dysregulation.6
Effective modifications begin with sensory considerations. Natural lighting, temperature control options, and acoustically managed spaces reduce physiological stress responses. Waiting areas designed with comfortable seating arrangements that allow personal space boundaries help survivors feel less exposed. The SAMHSA National Center for Trauma-Informed Care highlights environment as a key pillar of safety.
Privacy protections extend beyond confidentiality policies to physical design. Treatment spaces that prevent inadvertent exposure during vulnerable moments reinforce that safety is structural, not merely procedural. Facilities offering flexible scheduling options, including morning, afternoon, and evening sessions, recognize that survivors may need to avoid certain times or settings that carry triggering associations.
These environmental considerations integrate seamlessly with research-supported therapies like grounding skills and emotional regulation therapy, creating a cohesive treatment experience. When physical spaces align with therapeutic principles, survivors can focus cognitive resources on recovery work while minimizing environmental stress.
4. Transparent Communication Protocols
Establishing clear communication protocols creates predictability and safety throughout treatment. When individuals understand what information will be shared, who will have access to it, and how conversations will be structured, they can engage more fully in their recovery work. This transparency reduces anxiety and builds the trust necessary for meaningful therapeutic progress.7
Effective protocols begin with explicit consent practices. Before sharing any clinical information—even within the treatment team—staff should explain what will be discussed, why it matters for care, and who will be involved. Research published by the National Center for Biotechnology Information underscores the importance of transparent communication in preventing re-traumatization.
To standardize this across your facility, consider implementing specific communication scripts in your EHR system prompts:
// Standard Consent Introduction Script "Before we begin, I want to let you know how this information is used. I will take some notes today to help our clinical team coordinate your care. You have the right to review these notes at any time. Are you comfortable proceeding?"
Communication skills training within group settings also supports healing-centered care. Teaching specific techniques for giving and receiving feedback, setting boundaries, and expressing needs helps create a culture of mutual respect. These skills prove particularly valuable in structured day programs and hospital-based outpatient settings.
Documentation practices should be explained clearly as well. When clinicians discuss how session notes are recorded, what goes into treatment plans, and how progress is tracked, it demystifies the clinical process. Programs that integrate CBT and DBT can weave these communication principles throughout their curriculum, ensuring transparency becomes an ongoing practice.
5. Peer Support Integration
Peer support integration represents one of the most powerful elements of care that honors the impact of past experiences on recovery. Individuals who have navigated their own recovery journey bring unique insights that clinical training alone cannot replicate. Their lived experience creates an immediate foundation of credibility and understanding that can accelerate therapeutic progress for others facing similar challenges.8
Effective peer support programs operate within clearly defined boundaries that protect both supporters and participants. Certified peer recovery specialists receive training in maintaining appropriate professional relationships while sharing their experiences authentically. According to SAMHSA Behavioral Health Barometer reports, peer integration significantly boosts long-term recovery metrics.
Integration works best when peer supporters collaborate directly with treatment providers instead of functioning as separate entities. Regular case consultation ensures that peer interventions align with treatment goals and therapeutic approaches.
- Define Roles Clearly: Establish distinct boundaries between clinical therapy and peer support.
- Integrate into Care Teams: Include peer specialists in weekly clinical case reviews.
- Provide Ongoing Supervision: Ensure peer workers have access to clinical supervisors to process their own secondary trauma.
Programs like IOP and PHP benefit significantly from structured peer involvement. Peer supporters can facilitate group discussions, provide between-session check-ins, and help participants navigate practical recovery challenges. Their presence normalizes the recovery process and demonstrates that long-term wellness is achievable.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
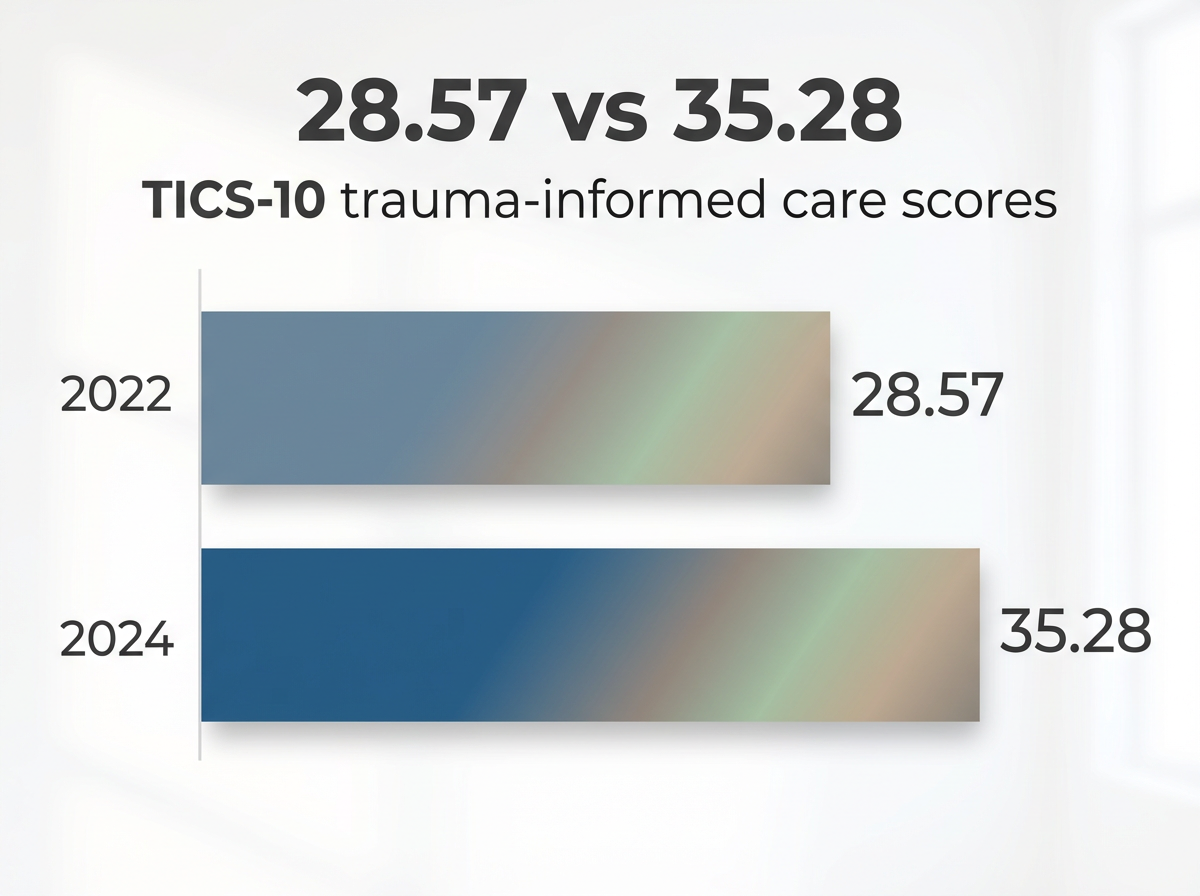
6. Staff Training and Secondary Trauma Prevention
Treatment providers working in trauma-informed environments face unique occupational hazards that extend beyond standard clinical challenges. Secondary traumatic stress—the emotional residue of exposure to others' trauma narratives—can compromise both staff wellbeing and the quality of care delivered. Effective trauma-centered programs recognize that protecting care teams is essential to sustaining compassionate, effective treatment.9
Comprehensive staff training addresses both trauma recognition and self-care practices. Care teams benefit from education on trauma neurobiology, attachment theory, and how past trauma manifests in treatment resistance or challenging behaviors. A study in Psychological Trauma: Theory, Research, Practice, and Policy confirms that supported staff yield better patient outcomes.
Organizations that prioritize staff wellness create sustainable trauma-aware cultures. Regular clinical supervision provides space for processing difficult cases and identifying signs of compassion fatigue. Peer consultation groups allow clinicians to share challenges and strategies without judgment. Some programs implement mandatory self-care protocols, recognizing that clinician wellness directly impacts treatment outcomes.
Coastal Recovery Partners integrates trauma-sensitive principles throughout clinical operations, including robust staff support structures. The facility's approach combines research-validated therapies like CBT and DBT with explicit trauma protocols, delivered by teams trained in recognizing both client trauma responses and their own secondary stress. This comprehensive model ensures that clinicians remain equipped to provide consistent, attuned care.
7. Integrated MAT with Trauma-Sensitive Protocols
Medication-assisted treatment (MAT) becomes significantly more effective when integrated with protocols that recognize the deep connections between traumatic experiences and patterns of dependency. Many individuals in recovery have used substances as a way to manage overwhelming emotions, intrusive memories, or physiological responses tied to past trauma. When MAT programs operate without awareness of these underlying wounds, they risk addressing only the biological aspects of addiction.10
Protocols sensitive to past trauma begin with understanding that medication stabilization creates a foundation for deeper therapeutic work. As medications like buprenorphine or naltrexone reduce cravings and withdrawal symptoms, individuals gain the emotional bandwidth to engage with therapies focused on processing difficult experiences. The National Institute on Drug Abuse emphasizes that MAT must be paired with comprehensive behavioral therapies for optimal trauma recovery.
The approach also demands modifications to standard MAT procedures. For survivors with medical trauma, the process of receiving injections or regular monitoring may trigger distress. Providers attuned to these sensitivities offer choices whenever possible, explain procedures thoroughly, and recognize that missed appointments may reflect survival responses more than lack of commitment.
Coastal Recovery Partners integrates medication-assisted treatment within comprehensive dual diagnosis care that addresses both chemical dependency and co-occurring mental health conditions through a lens that honors past wounds. Their coordinated approach combines MAT with proven therapies including CBT, DBT, and relapse prevention, delivered by clinicians trained to recognize how traumatic experiences shape recovery. This integration ensures that medication management supports the essential therapeutic work.
Remember that recovery is a journey of rebuilding trust—in yourself, in others, and in the process of healing. If you are ready to explore your options, reach out to Coastal Recovery today. We're here to help guide you toward a future defined not by your past, but by your resilience and hope.

Frequently Asked Questions
How were these seven trauma-informed care practices selected?
These seven trauma-informed care practices were chosen based on their alignment with core principles established by leading authorities, including safety, trustworthiness, peer support, collaboration, and empowerment. Each practice is supported by research showing its effectiveness in reducing treatment dropout rates and improving engagement—outcomes that are vital for trauma survivors in recovery. The selection process emphasized organizational strategies that are widely applicable, evidence-based, and adaptable across outpatient and intensive outpatient settings. By focusing on examples of trauma informed care that are practical for clinicians and administrators, this list reflects practices with strong empirical backing and real-world impact.1,3
What happens if trauma screening at intake reveals severe PTSD symptoms?
If trauma screening at intake reveals severe PTSD symptoms, the clinical team should respond with a trauma-informed approach—prioritizing safety, respect, and choice. Immediate steps include ensuring the individual feels supported and not rushed, collaborating on next steps, and assessing for risk factors such as suicidality or self-harm. Clinicians may recommend integrated treatment that addresses both substance use and PTSD, and if needed, provide referrals to specialized trauma therapy. Open communication and shared decision-making remain vital, as these are key examples of trauma informed care that prevent re-traumatization and support engagement.1
Can trauma-informed care be implemented effectively in outpatient settings?
Yes, trauma-informed care can be implemented effectively in outpatient settings. Outpatient programs are well-suited for examples of trauma informed care because they prioritize safety, transparency, and client empowerment throughout flexible, community-based services. Research shows that when outpatient teams integrate trauma-informed principles—such as universal trauma screening, collaborative treatment planning, and ongoing staff training—clients experience higher engagement and lower dropout rates compared to standard care models. These results are consistent across intensive outpatient and traditional outpatient programs, where building trust and preventing re-traumatization are essential. Organizational commitment—not the level of care—drives success in trauma-informed implementation.1,3
Why isn't specialized trauma therapy like EMDR included in this list?
Specialized trauma therapies like EMDR are highly effective but are not included in this list because the focus here is on core organizational practices that benefit all clients—not just those needing trauma-specific interventions. Trauma-informed care refers to a universal framework that shapes the environment, policies, and day-to-day interactions in treatment settings. Examples of trauma informed care emphasize safety, trust, and collaboration for everyone, regardless of trauma history, whereas EMDR is a targeted clinical intervention for processing trauma memories. National guidelines define trauma-informed care as a system-wide approach, not a specific therapy or treatment modality.1
How do trauma-informed practices address cultural differences in trauma experience?
Trauma-informed practices address cultural differences in trauma experience by prioritizing cultural humility, seeking to understand how trauma is shaped by identity, history, and community context. Providers are encouraged to recognize and respect unique cultural expressions of distress, coping, and healing. This means adapting assessments, communication styles, and interventions to fit each individual’s background. National guidelines recommend involving community members and using culturally responsive frameworks to avoid imposing a one-size-fits-all approach. Among the most effective examples of trauma informed care, culturally attuned practices help ensure safety and trust for clients from marginalized or historically oppressed groups.1
What measurable outcomes indicate successful trauma-informed care implementation?
Successful trauma-informed care implementation is reflected in several measurable outcomes. Key indicators include increased treatment engagement, lower dropout rates, and improved client satisfaction. Research consistently shows that organizations adopting trauma-informed frameworks see a 20-35% rise in engagement and a significant decline in early departures from treatment. Another crucial outcome is the strengthening of therapeutic alliance scores, which signal deeper trust between clients and providers. Additionally, staff report higher confidence and reduced burnout when trauma-informed practices are embedded into care environments. These outcomes confirm that authentic examples of trauma informed care translate into both better clinical results and healthier organizational cultures.3,4
References
- SAMHSA's Concept of Trauma and Guidance for a Trauma-Informed Approach. https://www.samhsa.gov/sites/default/files/dtap_files/samhsa_trauma_guidance_final.pdf
- National Institute on Drug Abuse: Substance Use and Trauma. https://www.nida.nih.gov/publications/research-reports/substance-use-in-women/substance-use-trauma
- Journal of Substance Abuse Treatment: 'Trauma-Informed Care in Addiction Treatment: Clinical Impact and Implementation'. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7225060/
- American Psychological Association: Understanding Trauma and Trauma Responses. https://www.apa.org/science/about/psa/trauma/index
- SAMHSA National Center for Trauma-Informed Care (NCTIC). https://www.samhsa.gov/nctic
- JAMA Psychiatry: 'Prevalence of Childhood Trauma in Substance Use Disorder Populations'. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5478079/
- National Center for Biotechnology Information: 'Substance Use, Abusive Relationships, and Intimate Partner Violence'. https://www.ncbi.nlm.nih.gov/books/NBK207191/
- Psychological Trauma: Theory, Research, Practice, and Policy: 'Trauma-Informed Care Reduces Re-traumatization and Improves Outcomes'. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4471340/
- National Institute on Drug Abuse: 'Substance Use Disparities and Trauma in Tribal Communities'. https://www.drugabuse.gov/sites/default/files/files/TribalSUDisparities.pdf
- SAMHSA Behavioral Health Barometer: State and National Trends. https://www.samhsa.gov/data/sites/default/files/report_3223/ShortReport-10-508.pdf





