Accessible Recovery Treatment in Portland, ME

Understanding Options for Recovery Treatment in Portland ME
Tool: Quick Level-of-Care Assessment
Before reading further, ask yourself these three questions to gauge where to start:
- Safety: Do I experience severe withdrawal symptoms (shaking, seizures) when I stop? (If yes, medical detox is the priority).
- Environment: Is my home free of substances and supportive of my sobriety? (If no, residential care may be safer).
- Obligations: Do I need to work or care for family during treatment? (If yes, IOP or Outpatient is designed for you).
When facing addiction, knowing what treatment options are available can feel overwhelming. The good news is that recovery treatment in Portland ME isn't one-size-fits-all, and understanding the different pathways can help you or your loved one find an appropriate fit for lasting healing.
Recovery programs generally fall into several categories, each designed to meet different needs and circumstances. To help you compare, we have broken down the primary options available locally:
Inpatient or residential treatment provides 24-hour care in a structured environment, offering intensive support for those who need to step away from daily triggers. This option works well for individuals with severe addiction or co-occurring psychological conditions. For example, someone with a decade-long opioid dependency and unstable housing might begin with 90-day residential treatment.
Outpatient programs allow individuals to receive treatment while maintaining work, school, or family responsibilities. These programs vary in intensity. A professional with recent alcohol misuse and strong family support, for instance, might start with intensive outpatient care that allows them to continue working while attending evening therapy sessions.
Detoxification services address the physical dependence on substances, providing medical supervision during withdrawal. This critical first step ensures safety and comfort as the body adjusts to functioning without drugs or alcohol.
Medication-assisted treatment (MAT) combines FDA-approved medications with counseling. This evidence-based approach has proven particularly effective for opioid and alcohol use disorders. Research shows that individuals receiving MAT are significantly more likely to remain in recovery compared to those receiving counseling alone.7
Self-Assessment: Is Outpatient Care Right?
A simple self-assessment can help you decide if outpatient care is a good match for your recovery journey. Start by checking off statements like: "I feel safe at home," "I can manage daily responsibilities," and "I have a stable support system." This approach is ideal for those who want to stay connected to work, family, or school while receiving treatment.
In Portland, outpatient recovery services offer evidence-based therapies, medication-assisted options, and trauma-informed care—supporting you in your daily life. Intensive outpatient programs (IOPs) and partial hospitalization programs (PHPs) are especially helpful for people seeking flexibility without stepping away from their community.9
Evaluating Your Current Stability Level
Use this quick checklist to gauge your current stability before considering outpatient recovery treatment in Portland ME:
- Do you feel physically safe at home?
- Are you free from immediate, dangerous withdrawal symptoms?
- Can you access reliable transportation to and from the center?
These questions can help clarify if outpatient addiction counseling or intensive outpatient programs are a good fit. This approach works best when you’re not experiencing severe withdrawal or acute mental health crises. About half of individuals with substance use challenges also have co-occurring mental health conditions, so integrated support is especially important during this stage.9
Assessing Daily Responsibility Commitments
Before committing to outpatient treatment, map out your daily responsibilities. List all fixed commitments (work shifts, caregiving, school hours, appointments) over a typical week. Are there blocks of time you can consistently dedicate to therapy sessions?
Many Portland outpatient programs offer evening or weekend options, making it easier for working adults and parents to attend without major disruptions. Integrated care that addresses both substance use and mental health is especially valuable, as nearly half of those in treatment juggle multiple responsibilities and co-occurring conditions.9
Treatment Intensity Levels Explained
To help you compare your options, list how many hours per week you could realistically dedicate to treatment, and note any support needs such as medical monitoring or mental health care. This will clarify which level of care fits your situation.
Partial Hospitalization vs IOP Programs
Partial Hospitalization Programs (PHP) generally require attendance five days a week for several hours each day, providing close medical and mental health monitoring. This approach works best when someone needs a high level of daily support but does not require overnight stays.
Intensive Outpatient Programs (IOP), by contrast, usually meet three to five times per week for shorter blocks, offering more flexibility for work or family life. Research shows that IOP outcomes are comparable to residential care for 80–90% of appropriate candidates, making it a strong choice for many in Portland.2
Standard Outpatient Support Structures
Standard outpatient programs usually involve one or two group or individual therapy sessions each week. This structure makes it easier for people with steady home environments or less intensive support needs to stay on track. These programs often include evidence-based counseling, medication management, and connection to peer support groups.
Decision Framework for Recovery Treatment in Portland ME
Tool: Treatment Priority Matrix
Rank the following factors from 1 (Low Priority) to 5 (High Priority) to see what your treatment plan must include:
- __ Mental Health: Do I need help with anxiety, depression, or trauma?
- __ Medication: Do I need MAT (Suboxone, Methadone, Vivitrol) to manage cravings?
- __ Schedule: Do I need evening/weekend hours to keep my job?
- __ Cost: Do I need a program that accepts my specific insurance (e.g., MaineCare)?
Choosing an appropriate treatment approach requires careful consideration of several interconnected factors. The decision isn't simply about selecting the most intensive option or the one that fits most conveniently into a schedule. Instead, it involves honestly assessing current circumstances.
The severity of substance use provides a starting point for evaluation. Someone experiencing severe withdrawal symptoms or medical complications needs a different level of support than someone with a milder dependency. Physical health considerations, co-occurring psychological conditions, and the presence of a supportive home environment all influence which treatment setting will be most effective.
Previous treatment experiences also inform the decision. If someone has attempted outpatient treatment multiple times without sustained success, a more structured environment might be necessary. Conversely, someone who has completed residential treatment and maintained stability might benefit from continuing care through outpatient services to reinforce progress.
Identifying Your Core Treatment Needs
Start with a practical worksheet: List your main treatment goals—such as managing anxiety or depression, seeking medication-assisted support, or needing trauma-sensitive care. This approach works best when you want to personalize your recovery treatment in Portland ME to address both substance use and any mental health needs.
Co-Occurring Mental Health Considerations
To determine if co-occurring mental health support should be a top priority, begin by listing any symptoms of depression, anxiety, ADHD, or past trauma alongside your substance use concerns. About half of all individuals seeking recovery treatment in Portland ME also face co-occurring mental health challenges, and outcomes are significantly better when both are addressed together.9
Integrated programs offer dual diagnosis care, meaning therapy and medication management can target both your substance use and mental health needs in one coordinated plan.
Medication-Assisted Treatment Benefits
MAT combines safe, FDA-approved medications like buprenorphine, methadone, or naltrexone with counseling to reduce cravings and withdrawal symptoms. This method is a strong fit for those with opioid or alcohol use disorder, especially if previous attempts at recovery were derailed by physical discomfort. Studies show that people receiving MAT perform significantly better on functional outcomes and are more likely to stay in treatment.7
Trauma-Informed Care Requirements
Trauma-informed care is a specialized approach that recognizes the strong connection between trauma and addiction, focusing on creating a safe, supportive environment and avoiding practices that might trigger distress. This method suits people who have a history of trauma, or who feel anxious or unsafe in traditional treatment settings.10
Practical Accessibility Factors
To make recovery treatment truly accessible, consider practical factors like scheduling and insurance. Can you attend sessions during typical work hours, or do you need evening or weekend options? Do you have reliable transportation, or would virtual sessions be helpful?
Scheduling Flexibility for Professionals
If you’re balancing a demanding work schedule, map out your typical workweek and highlight windows of time when you could consistently attend treatment—such as early mornings, lunch breaks, or after 5 p.m. Many local providers offer evening or weekend intensive outpatient and partial hospitalization programs, as well as telehealth options.
Insurance Coverage and Financial Planning
Begin by contacting your provider's admissions team—they can help verify your insurance benefits, outline what levels of care are covered, and explain any out-of-pocket expenses. Maine’s push for behavioral health parity aims to expand insurance coverage for addiction and mental health care, but many still encounter delays or gaps in payment.1
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Implementation Pathways by Situation
Tool: Readiness Checklist
Identify your current status to find your immediate next step:
- Acute Crisis: Suicidal thoughts or severe withdrawal? → Go to Emergency Room or Crisis Unit immediately.
- Stable but Struggling: Working but using substances daily? → Schedule an IOP assessment this week.
- Post-Rehab: Just finished inpatient? → Enroll in standard outpatient for maintenance.
Building on the decision framework outlined above, the path forward depends entirely on where someone finds themselves in their addiction journey right now. For those in acute crisis—experiencing suicidal thoughts, severe withdrawal symptoms, or complete inability to function due to substance use—immediate medical intervention provides the necessary foundation.
When the situation allows for planning but addiction symptoms remain severe, residential treatment centers create structured environments where recovery becomes the primary focus. These programs typically last 30 to 90 days and remove the substances, triggers, and enablers of daily life.
For individuals maintaining work or family responsibilities while struggling with substance dependence, intensive outpatient programs bridge the gap between full-time treatment and traditional weekly therapy. Meeting three to five times per week for several hours, these programs deliver substantial therapeutic support addressing addiction patterns while allowing people to sleep at home.
Starting Treatment for the First Time
If you’re starting recovery treatment in Portland ME for the first time, a clear path helps reduce anxiety. Begin with a simple decision tool: jot down your main concerns—such as substance use patterns, mental health symptoms, or recent life changes—then rank how much support you think you’ll need in each area.
What to Expect During Initial Assessment
During your initial assessment, you’ll meet with a compassionate admissions specialist or clinician who will guide you through a conversation about your substance use, mental health symptoms, and key life circumstances. Expect a warm, nonjudgmental atmosphere. Many Portland centers offer same-week assessments, so you can get started quickly.
Building Your Personalized Treatment Plan
Work step-by-step with your care team to outline your main priorities. Providers in Portland collaborate with you to choose the right mix of therapy (such as cognitive behavioral therapy or motivational interviewing), medication options, and support groups, all tailored to your unique situation.9
Transitioning from Higher Care Levels
If you’re stepping down from inpatient or hospital-based care, a structured transition plan is essential. Identify your primary needs post-discharge—such as ongoing therapy, medication management, or peer support groups—and create a weekly schedule for new appointments.
Step-Down Care Continuity Strategies
Providers in Portland coordinate step-down care by offering regular therapy sessions, medication management, and integrated mental health support. Since about 46% of substance use treatment centers now offer intensive outpatient programs, these community-based models provide a reliable bridge from hospital care to daily life.1
Maintaining Recovery Momentum at Home
A helpful tool for maintaining recovery momentum at home is a daily routine planner: jot down three healthy habits you want to keep—like attending therapy sessions, joining a virtual support group, or practicing mindfulness. Research shows that people who remain connected to treatment for 30 days or more have better abstinence rates.3

Your Next 30 Days Action Plan
Tool: 30-Day Roadmap
- Week 1: Call 2-3 providers, verify insurance, schedule assessment.
- Week 2: Complete assessment, tour facility (virtual or in-person), finalize work schedule adjustments.
- Week 3: Begin sessions, attend first group meeting, establish a "sober routine" at home.
- Week 4: Review progress with counselor, identify one peer support contact, adjust schedule if needed.
Breaking down your first month into manageable steps helps transform the overwhelming journey into recovery into achievable milestones. This timeline provides structure while remaining flexible enough to adapt to your unique situation and readiness for change.
Week 1-2: Research and Initial Contact
To get started with recovery treatment in Portland ME, begin your first two weeks with this checklist: gather your health insurance details, list your main priorities, and identify a few local providers. About half of individuals seeking substance use help also experience mental health challenges, so selecting a center that offers both is especially important for lasting recovery.9
Verifying Insurance and Program Fit
Contact your insurance provider or the admissions team at your preferred treatment center to confirm what levels of care—such as outpatient, IOP, or PHP—are covered. Ask about copays, deductibles, and any required pre-authorizations. Many centers in Portland will guide you through this process, offer help with paperwork, and explain coverage in plain language.
Scheduling Your Confidential Assessment
Once you’ve identified a few suitable providers, schedule your confidential assessment. Have your insurance information ready, note your main questions or concerns, and choose a contact method that feels comfortable—most centers accept phone calls, secure online forms, or even virtual intake appointments.
Week 3-4: Beginning Your Recovery Journey
During weeks three and four, your focus shifts to putting your treatment into practice. Start by establishing a steady routine: set reminders for therapy sessions, group meetings, or medication check-ins, and keep a journal of how you feel after each visit.
Establishing Your Treatment Routine
A daily routine planner is a practical tool to help you establish consistency. Start by scheduling your therapy sessions, group meetings, and any medication check-ins at set times each week. Research shows that remaining engaged for 30 days or more significantly increases abstinence rates.3
Building Your Support Network Early
Begin by listing people and groups who can help you feel understood—such as trusted friends, family members, or local support groups. Many Portland providers offer access to peer-led groups, family education sessions, and alumni programs, all designed to foster a sense of belonging.
Finding Compassionate Care in Portland
Choosing an appropriate treatment provider for a loved one represents one of the most important decisions families make. In Portland, families have access to compassionate professionals who understand that quality addiction treatment extends beyond addressing substance use—it's about restoring dignity, rebuilding connections, and supporting both clients and their families through the recovery journey.
At Coastal Recovery Partners, we take time to understand each person's unique story, circumstances, and recovery goals. We recognize that effective treatment plans adapt as needs change, whether that means adjusting therapy approaches, introducing new support services, or simply being present during difficult moments.
When you're ready to start your healthier path forward, start here.

Frequently Asked Questions
Choosing the right path to recovery often brings up important questions. Here are answers to common concerns about timing, costs, and effectiveness.
How effective is outpatient treatment compared to residential programs?
Outpatient recovery treatment in Portland ME is highly effective for many individuals, offering outcomes that closely match those of residential programs for most people. Research shows that intensive outpatient programs (IOPs) achieve similar results to inpatient care for 80–90% of appropriate candidates, with comparable reductions in substance use and strong abstinence rates. Outpatient options also allow you to maintain work, family life, and community connections while receiving care.2
What is the difference between IOP and PHP programs?
Partial Hospitalization Programs (PHP) typically require attendance five days a week for roughly 4-6 hours per day, offering intensive medical and mental health monitoring. Intensive Outpatient Programs (IOP) are more flexible, generally meeting three to five times a week for 3-hour sessions. PHP is often a step down from residential care, while IOP is ideal for working professionals needing structured support.2
Can I start treatment immediately, or is there a waiting list?
Many providers offering recovery treatment in Portland ME can schedule your first appointment within a week. Same-week assessments are common for outpatient and IOP services. While high-demand periods may cause short delays, contacting admissions teams directly often expedites the process. National data show that timely access is critical, as only about 23% of Mainers who need treatment receive it.6
What if I've tried treatment before and it didn't work?
Relapse does not mean failure; it often indicates a need to adjust the treatment plan. Many individuals require multiple episodes of care or a different level of intensity, such as moving from standard outpatient to an IOP. Providers in Portland offer evidence-based options like medication-assisted treatment (MAT) and trauma-informed care to address underlying issues that may have been missed previously.6
Are evening or weekend treatment options available for working professionals?
Yes, flexible scheduling is a hallmark of Portland's outpatient services. Many centers offer evening IOP sessions (e.g., 5:30 PM – 8:30 PM) and weekend groups to accommodate work and family commitments. Telehealth options are also widely available to reduce travel time, making it easier to balance employment with recovery.6
How confidential is my treatment information?
Your privacy is protected by strict federal (HIPAA, 42 CFR Part 2) and state laws. Information regarding your assessment, attendance, and progress cannot be shared with employers, family, or others without your specific written consent. Portland providers prioritize creating a safe, discreet environment.9
What ongoing support is available after I complete the program?
Post-treatment support, or aftercare, is crucial for long-term success. Local providers typically offer alumni groups, weekly check-in sessions, and connections to community peer support like AA, NA, or SMART Recovery. Engaging in aftercare for at least 30 days post-treatment significantly improves abstinence rates.3
Will I be able to keep my job while attending treatment?
Yes, most outpatient and IOP programs are designed to allow you to continue working. Employers may also be required to provide job protection under the Family and Medical Leave Act (FMLA) if you need to take time off for medical care. Discussing flexible hours with your employer and treatment team can help you balance both.9
What if I have both addiction and mental health challenges?
Approximately 50% of individuals seeking recovery also face mental health challenges like anxiety or depression. Integrated "dual diagnosis" programs in Portland address both conditions simultaneously through therapy and medication management, which is proven to yield better long-term results than treating them separately.9
How much does outpatient treatment cost, and will my insurance cover it?
Costs vary by intensity. Standard outpatient sessions may range from $100–$250 per session, while IOPs can cost $3,000–$5,000 per month without insurance. However, most Portland providers accept commercial insurance and Medicaid. Maine's parity laws aim to ensure behavioral health is covered comparably to physical health. Always verify benefits with the admissions team first.1
How long do I need to stay in treatment to see results?
Research indicates that staying engaged in treatment for at least 90 days yields the best outcomes. However, the specific duration depends on your progress. You might start with 4-6 weeks of IOP and then transition to several months of standard outpatient care for maintenance.3
Can I involve my family in my recovery process?
Family involvement is highly encouraged and linked to better retention rates. Most centers offer family therapy, education nights, and multi-family groups to help repair relationships and build a supportive home environment.3
What happens if I relapse during outpatient treatment?
Relapse is viewed as a setback, not a failure. Your team will help you analyze the trigger, adjust your treatment plan (potentially increasing intensity), and strengthen coping skills. You will generally not be expelled; instead, you will be supported in getting back on track.3
Is medication-assisted treatment right for me?
MAT is highly effective for opioid and alcohol use disorders. It combines FDA-approved medications (like buprenorphine or naltrexone) with counseling to reduce cravings and normalize brain chemistry. If you struggle with physical dependence or chronic relapse, MAT can stabilize you enough to engage fully in therapy.7
How do I know if a program is trauma-informed?
A trauma-informed program prioritizes safety, choice, and empowerment. Staff should ask about your history without forcing disclosure, avoid shaming language, and offer gender-specific or trauma-focused therapies. Ask specifically if their clinical team is trained in modalities like EMDR or trauma-focused CBT.10
References
- Clinical Issues in Intensive Outpatient Treatment (SAMHSA TIP 47). https://library.samhsa.gov/sites/default/files/pep20-02-01-021.pdf
- Substance Abuse Intensive Outpatient Programs (Journal of Substance Abuse Treatment). https://pmc.ncbi.nlm.nih.gov/articles/PMC4152944/
- Evidence-Based Practices for Substance Use Disorders (Clinical Psychology Review). https://pmc.ncbi.nlm.nih.gov/articles/PMC3678283/
- Efficacy of Cognitive Behavioral Therapy for Alcohol and Other Drug Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC9948631/
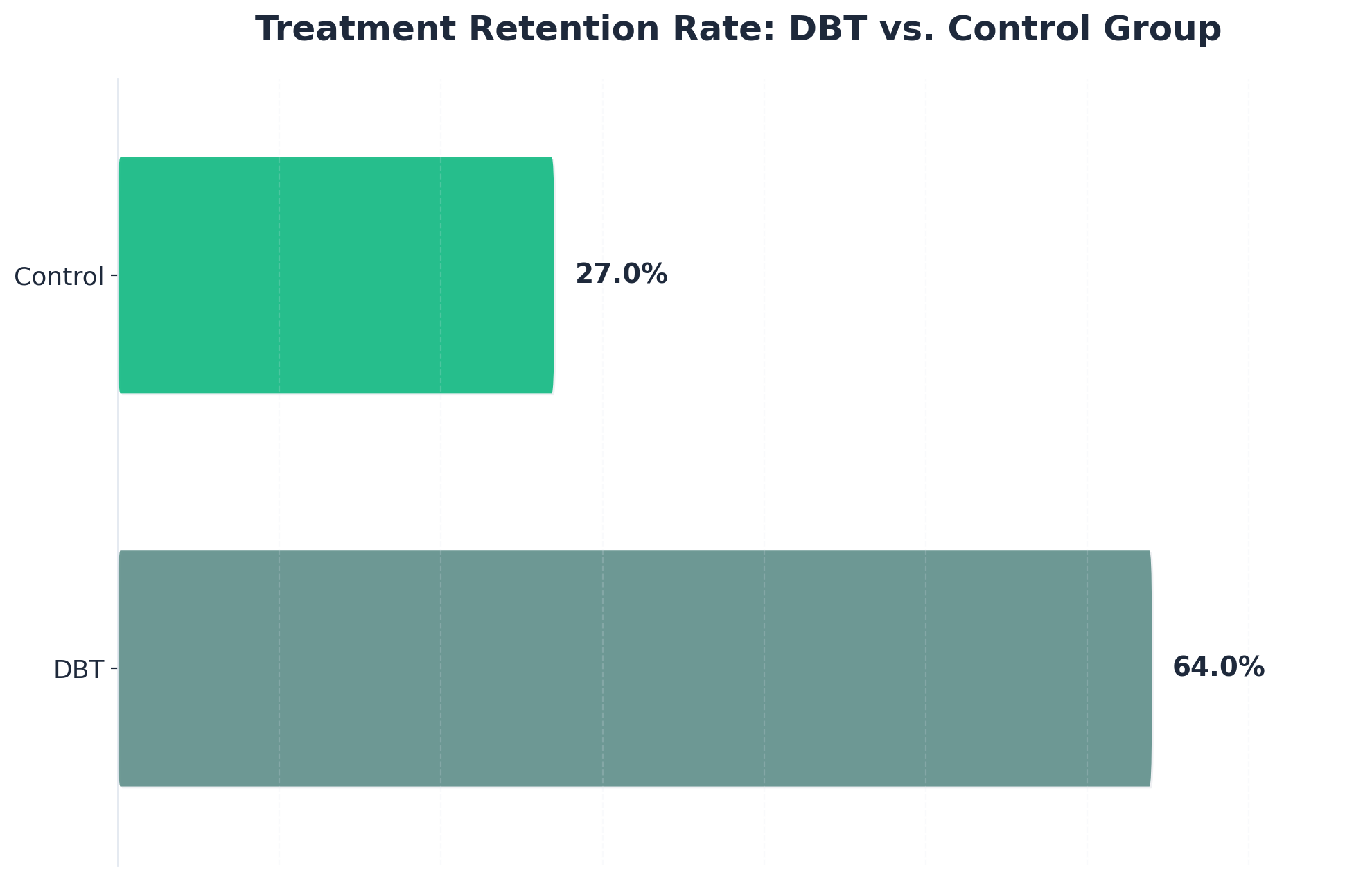
- Dialectical Behavior Therapy for Substance Abusers. https://pmc.ncbi.nlm.nih.gov/articles/PMC2797106/
- Using Motivational Interviewing in Substance Use Disorder Treatment (SAMHSA Advisory 35). https://library.samhsa.gov/sites/default/files/PEP20-02-02-014.pdf
- Effects of Medication-Assisted Treatment (MAT) for Opioid Use Disorder. https://pmc.ncbi.nlm.nih.gov/articles/PMC7302321/
- Effectiveness of Medication Assisted Treatment for Opioid Use in Prison and Jail Settings. https://www.chcs.org/resource-center-item/effectiveness-of-medication-assisted-treatment-for-opioid-use-in-prison-and-jail-settings-a-meta-analysis-and-systematic-review/
- Treatment for Substance Use Disorder With Co-Occurring Psychiatric Conditions. https://pmc.ncbi.nlm.nih.gov/articles/PMC6526999/
- Trauma-Informed Care for Substance Abuse Counseling (Hazelden Betty Ford). https://www.hazeldenbettyford.org/research-studies/addiction-research/trauma-informed-care





