How to Choose an IOP Addiction Treatment Near Me

Key Takeaways
- IOP at ASAM Level 2.1 runs 9 to 19 clinical hours weekly across roughly 90 days, letting you keep working or parenting while getting real clinical care 48.
- IOP isn't right for everyone. Active medical withdrawal, unsafe housing, or repeated relapses often call for detox, residential, or PHP first, since matching care to needs drives outcomes 7.
- Ask whether the program treats co-occurring mental health conditions under one roof using evidence-based therapies like CBT, DBT, and motivational interviewing, plus MAT when opioids or alcohol are involved.
- Confirm the program is licensed by Maine DHHS under 34-B MRS §3601 and §3603, names its clinicians' credentials, and uses ASAM-based biopsychosocial assessments 54.
- Get specific about weekly schedules, morning versus evening tracks, virtual options, and missed-session policies so treatment hours fit your actual life, not an idealized one.
- Request a free insurance benefits check up front, with deductibles, co-pays, and pre-authorized sessions in writing, and ask about sliding-scale fees if you're uninsured.
- Choose a program that plans the step-down from day one — ongoing therapy, alumni groups, MAT coordination, and a clinical relapse response rather than a discharge handshake.
Recovery That Fits Inside Your Actual Week
You're reading this because something has to change, and you're trying to figure out how to make that change without losing your job, your kids' bedtime routine, or whatever fragile structure is currently holding your week together. That's a reasonable thing to worry about. It's also not a reason to wait.
An Intensive Outpatient Program, or IOP, is built for exactly this moment. You live at home. You keep working, parenting, or going to school. You show up several days a week for therapy, group work, and skill-building, then you go back to your life and practice what you learned. For most people without a 24-hour medical need, research shows IOP can be as effective as residential treatment 6.
The hard part isn't deciding that you need help. You probably already know that. The hard part is choosing a program that's actually licensed, actually evidence-based, and actually fits the life you're trying to protect. Around South Portland and across Maine, the options can blur together quickly, and the marketing language on most websites won't tell you what really matters on a Tuesday at 6 p.m.
This guide gives you a clear, five-question framework you can use on your very first phone call. No jargon you don't need. No pressure. Just the questions that separate a credible IOP from a shaky one, so you can pick up the phone with your shoulders a little lower.
What an IOP Actually Looks Like (and Where It Sits on the Care Continuum)
IOP, PHP, and Standard Outpatient: The Real Differences
Before you can choose a program, you need a quick map of where IOP sits between the other options. Treatment isn't one thing. It's a stepladder, and IOP is the rung in the middle.
The clearest way to tell these levels apart is by how many clinical hours you spend in treatment each week. Under the American Society of Addiction Medicine (ASAM) framework, an Intensive Outpatient Program at Level 2.1 runs between 9 and 19 hours of clinical services per week 4. The widely cited minimum is 9 hours, usually split across three to five days, with a recommended duration of around 90 days 8. That's typically three group sessions a week, plus individual therapy, plus skill-building work like relapse prevention or emotional regulation.
A Partial Hospitalization Program (PHP) sits one rung up. You're still living at home, but you're in treatment most of the day, often 20 or more hours a week, five days a week. PHP is for people who need close clinical contact but don't require overnight medical supervision. Think of it as a day-program version of residential.
Standard outpatient is the rung below IOP. It usually means one therapy session a week, sometimes two, totaling under 9 hours. SAMHSA describes it as a coordinated mix of one-on-one and group work focused on coping skills 9. It's appropriate when you have stable footing and need ongoing support, not active stabilization.
If your last few weeks have felt like a slow-motion crisis but you don't need a hospital bed, you're probably looking at Level 2.1. That's the sweet spot IOP was designed for, and it's the level most South Portland adults end up in when they want serious clinical care without leaving their lives behind.

When IOP Is Not the Right Level of Care
Most articles about choosing an IOP skip this part because it complicates the pitch. You deserve the honest version. IOP is a strong fit for a lot of people, but not everyone, and walking into the wrong level of care can set your recovery back instead of forward.
IOP probably isn't the right starting point if you're still in active, medically risky withdrawal. Alcohol and benzodiazepine withdrawal in particular can be dangerous and sometimes life-threatening. If you've been drinking heavily every day or taking high-dose benzos, you likely need medical detox first, then a step down into IOP or PHP afterward. A reputable program will tell you this on the phone, not enroll you anyway.
It also isn't the right fit if your home environment makes sobriety nearly impossible right now. If the people you live with are using around you, if there's active violence, or if you have nowhere stable to sleep, the structure of IOP can't compete with what you're walking back into every night. Residential treatment or sober living plus outpatient care tends to work better in that situation.
And IOP may be too light if you've already tried it more than once and kept relapsing within days of starting. That's not a moral failure. It's clinical information. It often means you need either PHP, residential care, or a stronger medication-assisted treatment plan layered into your therapy.
On the other side, IOP can also be more than you need. If you've completed PHP or residential, have stable housing, and have been sober for a few months, standard outpatient or a strong aftercare track might be the better next step.
Research backs this matching principle directly: treatment outcomes improve when the level and type of care line up with the individual's specific problems and needs 7. The right question isn't "is this program good?" It's "is this program right for me, right now?" A solid admissions team will help you answer that, even if the answer points somewhere else.
The Five-Question Framework for Your 15-Minute Admissions Call
Most admissions calls last about 15 minutes. That's not a lot of time, and it's easy to come off the phone realizing you forgot to ask the things that actually matter. So here's a simple framework you can keep open on your phone or screenshot before you dial.
Five questions. That's it. Each one targets a different make-or-break factor in whether a program will work for you specifically — not for some abstract patient on a brochure. The framework is built around two ideas the research keeps coming back to: a program needs a real biopsychosocial assessment to place you correctly 4, and the care has to be matched to your particular problems and needs to actually work 7.
- Clinical Fit — Does what they treat match what you're carrying?
- Credentials — Are they licensed in Maine and staffed by qualified clinicians?
- Schedule — Will the hours fit your real week, not your ideal week?
- Cost — What will you actually pay, and what does insurance cover?
- Aftercare — What happens when the 90 days end?
The next five sections walk through each one, with the exact phrasing you can use on the call. Take notes. You're allowed to ask programs to slow down.
Question One: Does the Clinical Approach Match What You Actually Need?
This is the question most people skip, and it's the one that quietly determines whether a program will work for you. "Do you treat substance use?" isn't enough. Substance use rarely shows up alone, and the right IOP needs to be equipped for the whole picture you're walking in with.
Start with what you're actually carrying. Are you dealing with depression, anxiety, PTSD, or unprocessed trauma alongside the drinking or drug use? That's called a co-occurring or dual diagnosis, and it's common — not a complication you should feel embarrassed about. If a program treats substance use but hands the mental health piece off to someone else, you'll spend your week translating between two providers who don't talk. Look for a program that integrates dual diagnosis care under one roof, with clinicians trained to treat both at the same time.
Ask what therapies they actually use in group and individual sessions. The names you want to hear are evidence-based: cognitive behavioral therapy (CBT), dialectical behavioral therapy (DBT), motivational interviewing, and structured relapse prevention. If trauma is part of your story, ask whether the program is trauma-informed, meaning the staff is trained to avoid retraumatizing you in group settings and to pace exposure carefully.
If opioids or alcohol are part of your picture, ask whether they offer or coordinate medication-assisted treatment (MAT) — medications like buprenorphine or naltrexone paired with therapy. MAT isn't a moral question. It's a clinical tool, and a program that dismisses it outright is one to skip.
Here's the underlying principle, and it's well-established in the research: matching treatment to your particular problems and needs is one of the strongest predictors of whether care actually works 7. A solid program will start with a thorough biopsychosocial assessment — a structured intake covering your medical history, mental health, substance use patterns, family, work, and trauma history — before they ever quote you a schedule 4.
On the call, try this: "I'm dealing with [name what you're carrying — anxiety, trauma, alcohol, opioids, all of it]. Walk me through how your program would treat that specifically." If the answer is generic, keep calling. If they get specific about therapies, clinicians, and how the pieces connect, you've found something real.
Question Two: Is the Program Licensed and Credentialed in Maine?
This one is a hard gate, not a preference. If a program isn't properly licensed, nothing else on the brochure matters. Good news: it takes about ten minutes to check, and you can do it before your second phone call.
In Maine, substance use disorder treatment programs are licensed and overseen by the Department of Health and Human Services (DHHS) through its Division of Licensing and Certification. The agency licenses Mental Health and Substance Use Disorder programs under 34-B MRS §3601, §3603, and related statutes 5. State regulations also spell out specific requirements for things like methadone services, which must show documentation of SAMHSA, DEA, and state approval 10. Translation: a real Maine IOP can tell you, in plain language, who licenses them and under what authority. If the answer is vague, that's the answer.
On the call, you can ask three short things. "Are you licensed by Maine DHHS as a substance use disorder treatment program?" "Can you give me your license number or point me to where it's listed?" "Who are your clinicians, and what are their credentials?" You're looking for licensed clinical social workers (LCSW), licensed clinical professional counselors (LCPC), licensed alcohol and drug counselors (LADC), and a medical director who oversees any medication-assisted treatment.
Ask whether the program follows ASAM criteria. A licensed IOP should use a structured biopsychosocial assessment to confirm Level 2.1 is the right fit for you, not just enroll whoever calls 4. That assessment is a sign the program treats placement as a clinical decision, not a sales decision.
You don't need to memorize statutes. You just need to hear that a program knows its own license, names its clinicians, and uses standardized assessment tools. Anything less, keep dialing.

Question Three: Will the Schedule Survive Contact With Your Real Life?
This is where a lot of people get stuck. The clinical fit looks right, the program is licensed, and then you open your calendar and panic. When exactly are you supposed to fit nine to nineteen hours of treatment a week around a job, school pickup, or a second-shift schedule that doesn't bend?
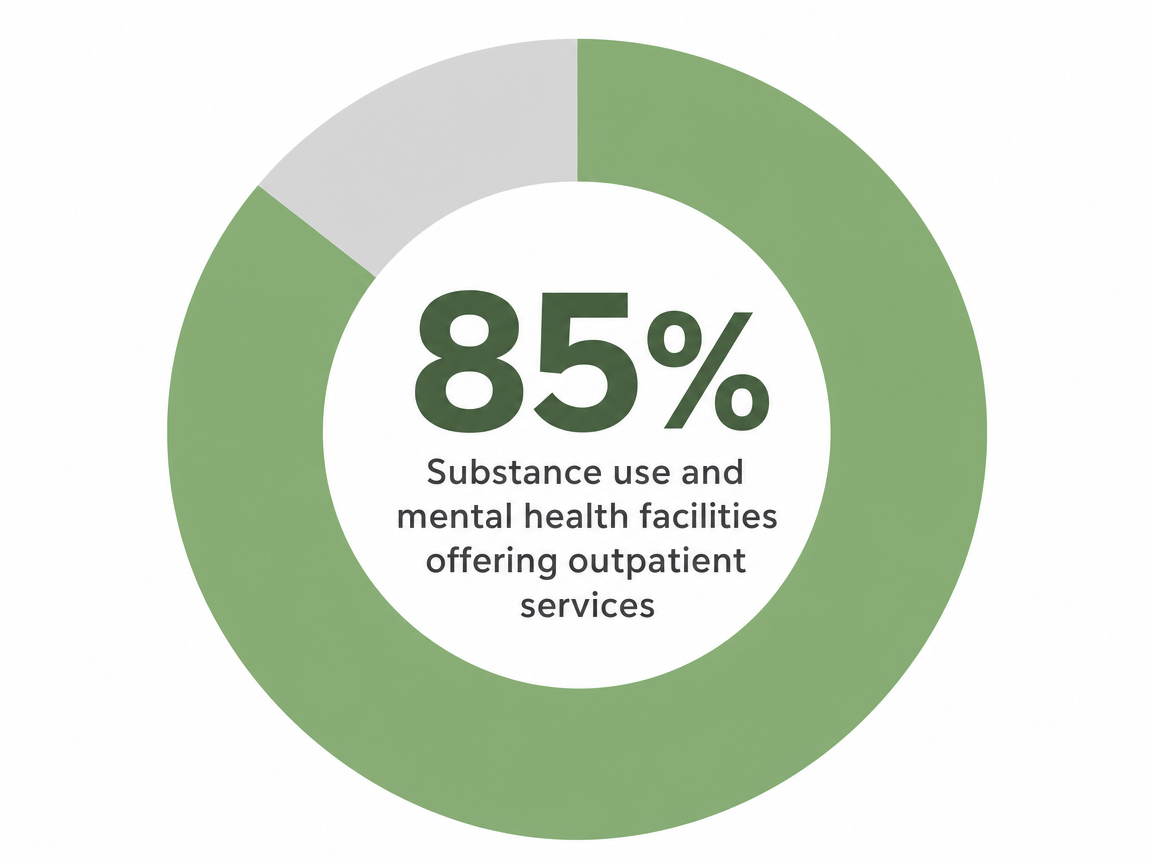
Here's the part that should ease your shoulders a little. Outpatient care is not some niche corner of the system. According to SAMHSA's 2024 N-SUMHSS report, 85% of US substance use and mental health treatment facilities offered outpatient services 1. That's the dominant form of care in this country, which means programs that schedule around working adults are common, not rare. You are not asking for special treatment by needing evening sessions.
On the call, get specific. Ask what days and times their IOP groups actually meet. A real Maine program will offer at least two scheduling tracks — typically a morning track for second-shift workers and parents with school-age kids, and an evening track for nine-to-fivers. If they only have one option and it doesn't fit, that's a no, not a maybe. Trying to white-knuckle a schedule that fights your life is a setup for dropping out in week three.
Ask the boring logistics too. How long is each session? Is anything offered virtually, and which sessions have to be in person? What's the policy when you have to miss a group for a sick kid or a work emergency? Is there a waitlist, or can you start within a week?
One more thing worth saying out loud: the Family and Medical Leave Act may protect time off for treatment if you've been at your job long enough, and many employers have employee assistance programs that handle this confidentially. You don't have to figure that out alone. A solid admissions team will help you think through it on the call.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Question Four: What Will This Cost, and What Does Your Insurance Actually Cover?
Money is the question that keeps people on the fence the longest, and it's the one programs are sometimes vaguest about. You deserve real numbers before you commit, not after.
Start by asking the program one direct question: "Do you accept my insurance, and can you run a benefits check before I enroll?" A solid admissions team will offer to verify your benefits for free, usually within a day or two. They'll come back with specifics — what your insurance covers for IOP at their facility, what your deductible is, what your co-pay or co-insurance per session looks like, and how many sessions are pre-authorized before they have to request more. Get those numbers in writing, even informally over email.
If you're insured through MaineCare, a commercial Maine plan like Anthem or Harvard Pilgrim, or a self-funded employer plan, ask whether the program is in-network. In-network means lower out-of-pocket costs. Out-of-network can still work, but you'll usually pay more, and you want to know that going in.
If you're uninsured or underinsured, ask two more things. "Do you offer a sliding-scale fee based on income?" and "Do you help with payment plans?" Many licensed Maine programs do, because the alternative is people walking away from care they need. There's no shame in asking. It's a normal admissions conversation.
One quiet cost worth naming: time off work, gas to and from sessions, childcare during groups. Build those into your math too. A program close to home in South Portland with flexible hours often costs less in real life than a cheaper program an hour away.
If a program won't talk specifics about cost on the first call, that's a flag. Treatment is expensive, but it shouldn't be a black box.
Question Five: What Happens After the 90 Days?
Here's a quiet truth most programs won't lead with: the work doesn't end when IOP ends. The recommended duration of intensive outpatient is around 90 days 8, but those three months are a launchpad, not a finish line. The right program treats them that way from day one.
Ask, on the call, what the step-down plan looks like. A real answer sounds something like: "Most clients move from IOP into our standard outpatient track for ongoing therapy, then into alumni support and aftercare groups as they stabilize." That's a continuum. What you don't want is a program that drops you off a cliff at week 13 with a handshake and a list of phone numbers.
Get specific about a few things. Will you keep the same individual therapist when you step down, or do you start over with someone new? Are there alumni groups, weekly check-ins, or a relapse-response protocol if you stumble? Does the program coordinate with your primary care doctor, your psychiatrist, or your MAT prescriber so the medication piece doesn't fall apart in the handoff? Recovery planning isn't a one-page discharge summary. It's a living plan that names the specific people, appointments, and supports that will hold you in month four, month six, and month twelve.
If you ever relapse — and many people do, at least once — ask what happens next. A good program treats a relapse as clinical information, not a reason to drop you. They re-assess, adjust the plan, and sometimes step you back up to PHP or detox briefly before returning to outpatient. That's not failure. That's how chronic conditions get managed.
Choose a program that's already thinking about month four when you're still in week one. That's the one that's actually planning to keep you well.
The Phone Screen Script You Can Use Today
Here's the script. Open your notes app, copy it down, and have it in front of you when you dial. You don't have to sound polished. You're allowed to read straight from the page.
- "I'm looking into IOP for myself. Can you tell me what you treat and whether you handle co-occurring mental health conditions like anxiety, depression, or trauma in the same program?"
- "Are you licensed by Maine DHHS, and what credentials do your clinicians hold?"
- "What does your weekly schedule look like? Do you have morning and evening tracks?"
- "Do you accept my insurance, and can you run a free benefits check before I commit?"
- "What therapies do you actually use — CBT, DBT, motivational interviewing? Do you offer or coordinate medication-assisted treatment if I need it?"
- "What does the step-down plan look like after IOP? Alumni groups, ongoing therapy, relapse response?"
- "How soon can I start?"
Seven questions. Take notes on the answers. If a program rushes you, dodges specifics, or pressures you to enroll today, hang up. The right program will slow down with you.
Making the Call When Everything in You Wants to Wait
You've read this far, which means part of you has already decided. The rest of you is just trying to find a reason to wait until Monday, until after the holiday, until the project at work wraps up. That voice is loud, and it's lying. There is no clean week coming. There is only this one, and the small, brave thing you can do inside it.
Making the call doesn't commit you to anything. It's a 15-minute conversation. You can use the script. You can take notes. You can hang up and call somewhere else. The point isn't to find the perfect program on the first try. The point is to start gathering real information instead of imagined worst-case scenarios.
If you're in or near South Portland, Coastal Recovery Partners is one of the local options worth putting on your list when you're ready to dial. Whoever you call first, call someone today. You've already done the hardest part, which was admitting this needed to change. The next step is just one phone number.
.webp)
Frequently Asked Questions
How many hours per week does an IOP require?
An IOP at ASAM Level 2.1 typically runs between 9 and 19 clinical hours per week 4. Most programs land near the 9-hour minimum 8, usually three group sessions plus individual therapy, spread across three to five days. That structure is what lets you keep working or parenting while still getting real clinical care. Ask the program for their exact weekly schedule before you commit.
How is IOP different from PHP and standard outpatient treatment?
The fastest way to tell them apart is hours. PHP is roughly 20 or more clinical hours a week, almost a full daytime schedule. IOP runs 9 to 19 hours weekly 4, usually in morning or evening blocks. Standard outpatient is under 9 hours, often just one or two therapy sessions a week focused on coping skills 9. IOP is the middle rung, designed to hold both treatment and your daily life.
How do I know if IOP is the right level of care for me?
You'll know during the assessment. A licensed program runs a structured biopsychosocial intake covering your medical history, mental health, substance use, and home environment to confirm Level 2.1 fits 4. IOP works well if you don't need medical detox, have a relatively stable place to sleep, and want clinical care without leaving your life. If withdrawal is medically risky or home isn't safe, you likely need a higher level first.
How long does an IOP program typically last?
The recommended minimum duration is around 90 days 8. Some people stay longer based on their progress and clinical needs, and some step down sooner into standard outpatient with continued therapy. Length isn't a finish line, it's a clinical decision your treatment team makes with you. Ask any program how they decide when you're ready to step down, and what aftercare or alumni support continues after the IOP phase ends.
How do I verify that an IOP is properly licensed in Maine?
Maine DHHS, through its Division of Licensing and Certification, licenses substance use disorder programs under 34-B MRS §3601, §3603 and related statutes 5. Programs offering methadone or related services must also document SAMHSA, DEA, and state approval 10. On the call, ask directly: are you licensed by Maine DHHS, and what's your license number? A real program will answer plainly. You can cross-check on the DHHS website.
Can I keep my job while attending an IOP?
Yes, that's exactly what IOP is built for. Most South Portland programs offer morning or evening tracks so you can fit treatment around a work schedule. Outpatient care is the dominant form of treatment in the country, with 85% of US substance use and mental health facilities offering it in 2024 1. The Family and Medical Leave Act and employee assistance programs may also protect or support your time. Ask about both.
References
- 2024 Data on Substance Use and Mental Health Treatment Facilities. https://www.samhsa.gov/data/report/2024-n-sumhss-annual-report
- Appendix B. Urine Collection and Testing Procedures and Alternative Methods for Monitoring Drug Use. https://www.ncbi.nlm.nih.gov/books/NBK64092/
- SAMHSA Releases Annual National Survey on Drug Use and Health. https://www.samhsa.gov/newsroom/press-announcements/20250728/samhsa-releases-annual-national-survey-on-drug-use-and-health
- LEVEL 2.1 INTENSIVE OUTPATIENT SERVICES BY SERVICE CHARACTERISTICS. https://www.pa.gov/content/dam/copapwp-pagov/en/ddap/documents/documents/asam/level%202.1%20by%20service%20characteristics.pdf
- Behavioral Health - Division of Licensing and Certification - Maine.gov. https://www.maine.gov/dhhs/dlc/licensing-certification/behavioral-health
- Substance Abuse Intensive Outpatient Programs: Assessing the Evidence. https://pmc.ncbi.nlm.nih.gov/articles/PMC4152944/
- Meta-Analyses of Seven of NIDA's Principles of Drug Addiction .... https://pmc.ncbi.nlm.nih.gov/articles/PMC3290709/
- Conceiving of a Continuum of.... https://www.ncbi.nlm.nih.gov/books/NBK64088/
- Treatment Types for Mental Health, Drugs and Alcohol | SAMHSA. https://www.samhsa.gov/find-support/learn-about-treatment/types-of-treatment
- 14-118 C.M.R. ch. 5, § 19 - SUBSTANCE ABUSE TREATMENT. https://www.law.cornell.edu/regulations/maine/14-118-C-M-R-ch-5-SS-19




