Recognizing Opioid Addiction Symptoms in a Loved One

Understanding Opioid Addiction Symptoms and Brain Chemistry
For decades, addiction was misunderstood as a moral failing or a lack of willpower. Today, medical research has definitively shown that recognizing opioid addiction symptoms early is critical because addiction is a chronic brain disease that fundamentally changes how the brain functions. This understanding is crucial for anyone seeking help or supporting a loved one through recovery.
When someone uses opioids repeatedly, these substances hijack the brain's reward system. Opioids flood the brain with dopamine, creating intense feelings of pleasure and relief. Over time, the brain adapts to these artificial surges by producing less dopamine naturally and reducing the number of receptors that can receive it. This neurological change means that everyday activities that once brought joy—spending time with family, enjoying a favorite meal, or pursuing hobbies—no longer provide the same satisfaction.
Impact on Brain Function
The encouraging news is that the brain can heal. With proper treatment and support, neural pathways can rebuild and restore healthier functioning. Evidence-based approaches including medication-assisted treatment, counseling, and comprehensive support services address both the physical and psychological aspects of this disease.
Physical Dependence vs. Addiction: Key Differences
To help families navigate the difference between physical dependence and addiction, use this quick checklist. Does your loved one take opioids as prescribed, or do they continue using despite harm? Physical dependence means the body adapts to a medication, leading to withdrawal symptoms if use stops. Addiction, however, involves compulsive drug-seeking and continued use regardless of negative effects on health, work, or relationships.5
Recognizing this distinction is key when looking for opioid addiction symptoms—dependence can occur even with proper use, while addiction signals a deeper behavioral change. Our team provides assessments and education to clarify these differences and guide the next steps for those seeing warning signs such as escalating cravings or loss of control.
How Tolerance Develops Over Time
Tolerance is when the body becomes used to a certain dose of opioids, so a person needs more of the drug to feel the same effect. This gradual increase often leads to using higher amounts or taking medication more frequently—an early warning sign when tracking opioid addiction symptoms. Tolerance develops because repeated opioid use changes how the brain and nervous system respond to pain and pleasure.5
Withdrawal Symptoms That Signal Dependence
When a loved one becomes physically dependent on opioids, withdrawal symptoms often appear if they miss a dose or try to stop. Signs may include:
- Muscle aches and tremors
- Runny nose and sweating
- Nausea, vomiting, and diarrhea
- Dilated pupils
- Insomnia and restlessness
These are among the most common opioid withdrawal symptoms. Family members might notice these discomforts emerging between doses, which can sometimes be mistaken for the flu. Our clinical team helps families understand these withdrawal warning signs and offers safe, medical support for managing withdrawal and preventing relapse.7
The Opioid Epidemic's Impact on Families
The opioid epidemic reaches far beyond individuals, deeply affecting families and entire communities. When someone experiences opioid addiction symptoms, loved ones often face emotional stress, financial strain, and uncertainty about how to help. National data shows that nearly 80,000 opioid-involved overdose deaths occurred in 2023, representing 76% of all drug overdoses in the U.S..7
Current Overdose Statistics and Trends
Assessment Tool for Families: Review the latest trends by asking—Has there been a change in overdose rates this year? Are new substances impacting your community? While 2023 marked the first annual decline in opioid deaths since 2018—with a 4% decrease from 2022—opioid addiction symptoms remain widespread, and synthetic opioids like fentanyl continue to drive risk. Families may also hear about xylazine entering the drug supply, which complicates overdose response.2
Why Early Recognition Saves Lives
Quick Response Checklist: If you notice early opioid addiction symptoms—such as sudden behavioral changes or unexplained physical issues—act promptly. Early recognition is vital, as most overdose deaths are preventable when someone intervenes quickly. The National Harm Reduction Coalition notes that it is rare for someone to die immediately from an opioid overdose, and survival often depends on timely help.6,7
Self-Assessment: Identifying Opioid Addiction Symptoms
Recognizing the early warning signs of opioid addiction in a loved one can be challenging, especially when denial or secrecy are involved. However, certain behavioral, physical, and lifestyle changes often signal a growing problem that requires attention and support.
Behavioral Changes That Signal Addiction
A practical self-assessment for families involves watching for behavioral changes like secrecy, sudden shifts in mood, or neglect of daily responsibilities, as these are common opioid addiction symptoms. You might notice your loved one withdrawing from social activities, losing interest in hobbies, or frequently missing work or school. Our team can help families interpret these changes and provide support, including confidential evaluations.1
Mood Swings and Personality Shifts
Frequent mood swings or sudden shifts in personality are often early opioid addiction symptoms. Loved ones might notice extremes—such as bursts of anger, irritability, or euphoria followed by deep sadness or withdrawal. According to Mayo Clinic, changes in mood, including swings from joy to anger, are common signs of opioid misuse.1
Changes in Daily Routines and Responsibilities
Disrupted routines—like missing work, skipping family events, or neglecting household chores—can be key opioid addiction symptoms. Loved ones may start sleeping at odd hours, forgetting important obligations, or letting bills and personal hygiene slide. These daily life changes often signal a shift in priorities, as opioid misuse begins to overshadow regular responsibilities.1
Doctor Shopping and Medication Misuse Patterns
"Doctor shopping"—visiting multiple healthcare providers to obtain extra prescriptions—or misusing medication by taking higher doses than prescribed are clear behavioral opioid addiction symptoms. These patterns are often paired with secrecy, lost or stolen prescriptions, or frequent requests for early refills.1
Physical Symptoms to Watch For
Physical symptoms are just as important as behavioral changes when it comes to identifying opioid addiction symptoms. Families can use this quick assessment:
- Are you noticing pinpoint pupils?
- Is there slowed breathing or unexplained drowsiness?
- Are there sudden weight changes?
- Do you see flushed skin or visible track marks?
These signs are common physical indicators of opioid misuse. Our medical team is equipped to evaluate these physical warning signs and offer clear, supportive next steps.1
Visible Signs: Pupils, Skin, and Appearance
Practical Tool: Check for pinpoint pupils (very small, constricted pupils), as this is a classic sign of opioid use and often appears even in well-lit environments. Other visible symptoms include flushed or unusually pale skin, unexplained bruises, or frequent scratching that leads to skin irritation. Some individuals may show sudden weight changes or appear disheveled, with poor hygiene or neglected grooming routines.1
Overdose vs. High Intoxication Indicators
It can be difficult to tell the difference between a loved one who is highly intoxicated on opioids and someone experiencing a life-threatening overdose. Use this comparison:
According to the National Harm Reduction Coalition, immediate action is critical if someone is hard to wake, not breathing normally, or their skin color changes.6
Emerging Concerns: Xylazine and Fentanyl
Families are now facing new challenges as illicit opioids are increasingly mixed with substances like fentanyl and xylazine. Fentanyl is 50 to 100 times more potent than morphine and is now a main driver of overdose deaths. Xylazine, a veterinary sedative, is sometimes added to street fentanyl, leading to additional physical signs such as unusually slow breathing, dangerously low heart rate, and skin ulcers that are slow to heal.4,8
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Addressing Opioid Addiction Symptoms: When to Intervene
Recognizing warning signs is an important first step, but knowing when to take action can feel overwhelming. With opioid use disorder, the decision to seek help doesn't require waiting until a crisis occurs—though the risk of overdose means timing is genuinely critical. Early intervention often leads to better outcomes and can prevent life-threatening situations from developing.
Consider reaching out for professional support when opioid use patterns persist for more than two weeks, daily functioning becomes impaired, signs of tolerance or withdrawal appear, or when the person is using opioids in dangerous situations. These aren't arbitrary markers—they represent points where professional guidance can make a meaningful difference in recovery trajectory and potentially save a life.
Assessing Severity Using Clinical Criteria
Practical Tool: Use the clinical severity checklist to gauge how serious opioid addiction symptoms have become. Experts rely on the DSM-5 criteria. If you answer "Yes" to two or more of the following within a 12-month period, it suggests opioid use disorder:5
- Taking larger amounts than intended?
- Persistent desire or unsuccessful efforts to cut down?
- Spending a lot of time obtaining, using, or recovering from the drug?
- Craving or strong urge to use opioids?
- Recurrent use resulting in failure to fulfill major role obligations?
- Continued use despite social or interpersonal problems?
Our clinical team conducts thorough assessments using these standards, helping you understand risk and guiding you toward appropriate treatment resources.
Understanding Co-Occurring Mental Health Issues
Co-occurring mental health issues—such as depression, anxiety, or bipolar disorder—often appear alongside opioid addiction symptoms. Many people with substance use disorders also experience other mental health challenges, and these can worsen cravings, withdrawal symptoms, and risk-taking behaviors. Our clinical team performs thorough screenings to identify both opioid misuse and mental health symptoms, offering integrated care plans that address the full picture.10
Approaching Your Loved One With Compassion
Having a compassionate approach is vital when addressing opioid addiction symptoms with a loved one. Start with an empathy checklist: Are you prepared to listen without judgment, use supportive language, and avoid blame? Taking these steps creates a safe space for open dialogue and increases the chances that your loved one will feel heard and understood.1
Communication Strategies That Work
Families often feel nervous about starting a conversation. Here’s a simple communication tool: begin by sharing your observations without judgment.1
"I’ve noticed you seem more withdrawn and missing work lately, and I'm worried about you."
The Mayo Clinic recommends listening calmly, expressing concern, and avoiding blame, as these techniques can lower defensiveness and encourage honest dialogue.
Crisis Resources and Immediate Support
In a crisis, quick access to support can make all the difference. If you notice overdose warning signs—like unresponsiveness, slow or irregular breathing, or blue-tinged lips—call 911 immediately and stay with your loved one while waiting for help. Families can also reach the SAMHSA National Helpline at 1-800-662-HELP (4357) for free, confidential guidance.3,6
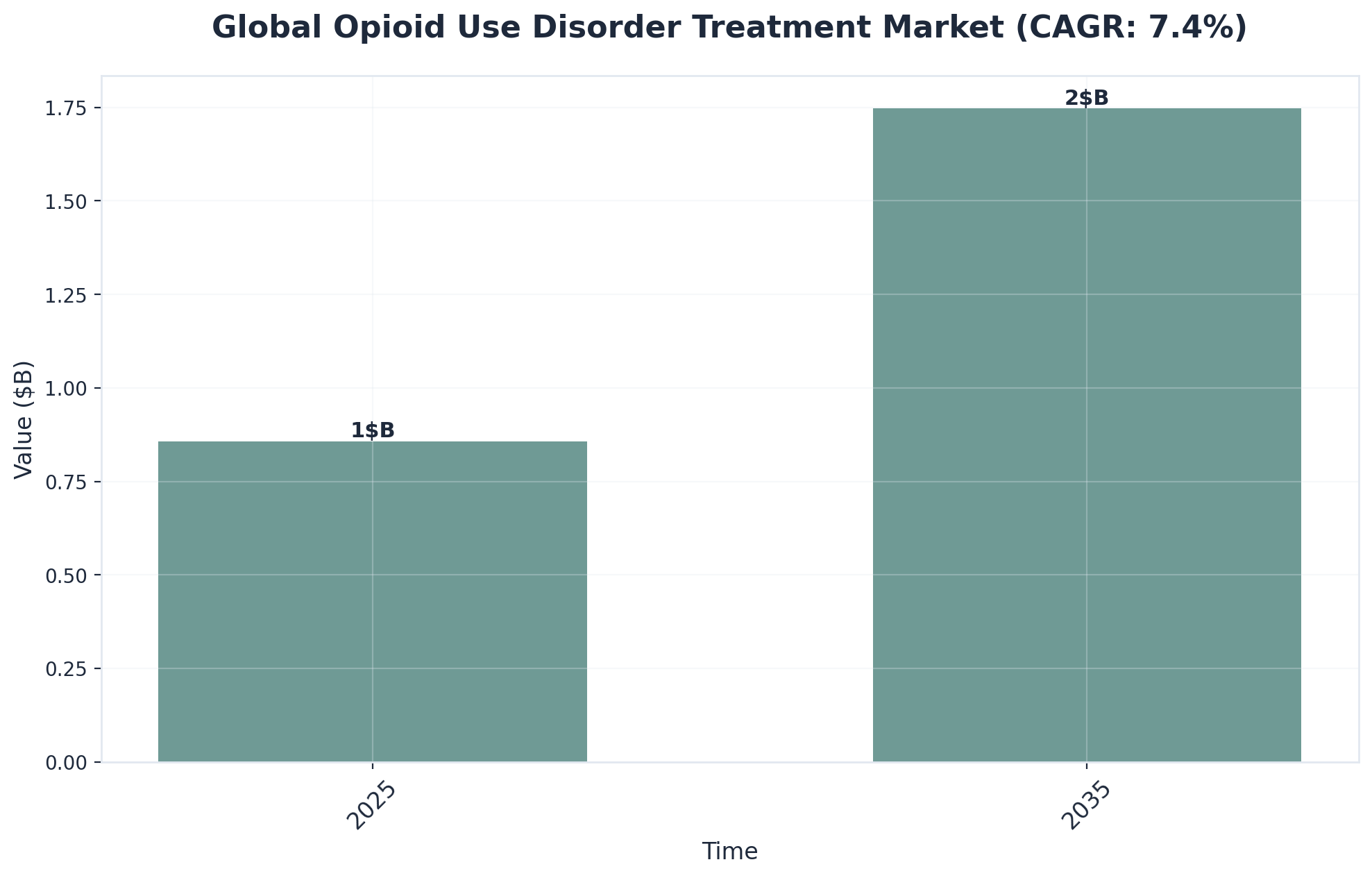
Implementation Pathways: Treatment Options
Once the decision to seek help has been made, understanding the available treatment pathways makes the journey forward less overwhelming. Professional support for opioid use disorder comes in several forms, each designed to meet different needs and circumstances while addressing both the physical and psychological aspects of addiction.
Outpatient vs. Residential Care Considerations
Use this simple decision checklist: Does your loved one have stable housing and a strong support system, or do they need 24-hour supervision to manage opioid addiction symptoms? Outpatient care lets individuals live at home while attending therapy and medication visits, offering flexibility for those with work or family commitments. Residential treatment provides round-the-clock structure and support.5
When Outpatient Programs Offer the Right Fit
Decision Checklist: Outpatient programs tend to offer the right fit when:
- Opioid addiction symptoms are moderate.
- Daily routines (work/school) remain mostly intact.
- There is strong support at home.
- The individual does not require 24-hour medical supervision.
According to Yale Medicine, outpatient treatment is effective for many with opioid use disorder, especially when early intervention occurs. Our outpatient services include individualized therapy, medication management, and family support sessions.5
Medication-Assisted Treatment Benefits
If your loved one shows opioid addiction symptoms such as strong cravings, withdrawal discomfort, or repeated relapse, medication-assisted treatment (MAT) may offer needed stability. MAT combines FDA-approved medicines like buprenorphine or methadone with counseling. Research shows MAT helps people stick with treatment longer and significantly lowers both opioid use and overdose deaths.5
Trauma-Informed and Dual Diagnosis Approaches
If your loved one’s opioid addiction symptoms are shaped by past trauma or come alongside mental health conditions like depression or anxiety, look for programs that offer trauma-informed care and dual diagnosis treatment. Dual diagnosis treatment addresses both opioid use warning signs and co-occurring mental health disorders in one coordinated plan, which research shows leads to better outcomes than treating each separately.5
Resource Planning for Recovery Success
Resource Planning Checklist: As your family confronts opioid addiction symptoms in a loved one, consider three pillars for recovery success:9
- Finances: Gather insurance information and explore coverage details.
- Family Involvement: Plan for active family participation in therapy.
- Relapse Prevention: Build a strategy with aftercare resources.
Research shows that family involvement can reduce substance use frequency by about 5.7%, or three fewer weeks of drug use each year.
Insurance Coverage and Financial Navigation
Start by gathering all insurance cards and calling your provider to confirm which opioid addiction symptoms and treatments are covered. Many families discover that coverage often includes outpatient therapy, medication-assisted treatment, and sometimes residential programs, but pre-authorization is commonly required. Our team can help you navigate the insurance process, answer benefit questions, and connect you with financial counseling.5
Your Next 30 Days: Taking Action Today
The next 30 days represent a critical window for establishing sustainable habits that support long-term opioid recovery. Rather than viewing this timeframe as overwhelming, breaking it into manageable weekly goals creates momentum.

Week 1-2: Documentation and Assessment
Practical Tool: Start a daily journal to document any behavioral changes, medication use patterns, and physical symptoms related to opioid addiction symptoms. Make simple notes about:
- Missed work or obligations
- Increased secrecy
- Mood shifts
- Visible signs like pinpoint pupils or drowsiness
Recent guidance highlights that family member observations are now routinely used by healthcare providers to identify opioid misuse earlier, making your documentation especially valuable1.
Week 3-4: Outreach and Treatment Connection
Outreach Checklist: Review your journal for patterns in opioid addiction symptoms, then take the next step by reaching out to trusted professionals. This stage often involves calling a treatment provider, scheduling a confidential assessment, or connecting with a support group for guidance. Healthcare teams now regularly encourage families to share their documented substance use warning signs, as these details help identify opioid misuse earlier and personalize care.1
Finding Compassionate Care in South Portland
When a loved one is struggling with opioid addiction, finding a treatment program that combines clinical expertise with genuine compassion makes all the difference. South Portland offers families access to evidence-based opioid addiction treatment services designed to support individuals through every stage of recovery.
The right treatment program creates an environment where patients feel safe, respected, and understood. Trained addiction specialists who understand the complexities of opioid use disorder recognize the unique challenges families face and provide personalized support that addresses both the physical and psychological aspects of addiction. From medically supervised detoxification to medication-assisted treatment (MAT) and comprehensive counseling, quality programs address the whole person—not just the substance use.
Conclusion
Taking this important step toward finding the right opioid addiction treatment doesn't have to feel overwhelming. National resources like SAMHSA's National Helpline (207) 835-3449 and local addiction treatment centers, such as Coastal Recovery Partners, can help you or your loved one heal and reclaim a happy, healthy, and fulfilling life.
You don't have to have all the answers. You just need to recognize the need for change. Connect with us today for free benefits verification and a personalized path forward.
.webp)
Frequently Asked Questions
When searching for opioid addiction support, many people have similar concerns and questions. Understanding what to expect can help ease some of the anxiety around taking that first step toward recovery.
How can I tell if my loved one is just dependent on prescribed opioids versus truly addicted?
Distinguishing between physical dependence and true opioid addiction symptoms can feel confusing, especially if your loved one uses prescribed medication. Dependence simply means the body has adapted to the medication, causing withdrawal symptoms if use stops. In contrast, addiction (opioid use disorder) involves behavioral changes: your loved one may continue using opioids despite harm, struggle to cut back, or show compulsive drug-seeking behaviors. If you see escalating cravings, doctor shopping, secrecy, or neglect of daily responsibilities, these are strong substance use warning signs that point beyond dependence alone.5
How do I know if an outpatient program will be enough or if residential treatment is needed?
Deciding between outpatient care and residential treatment depends on the severity and stability of your loved one's opioid addiction symptoms, their living situation, and the support they have at home. Outpatient programs are often enough if symptoms are moderate, routines are still manageable, and there’s a safe, supportive environment. However, residential treatment is usually needed for more severe substance use warning signs, repeated relapses, strong cravings, or when 24-hour supervision and structure are essential for safety and successful recovery.5
What happens if my loved one relapses after completing treatment?
Relapse after treatment is not a sign of failure, but rather a common part of the recovery journey for many facing opioid addiction symptoms. Because opioid use disorder is a chronic condition, setbacks can occur. If your loved one returns to substance use, look for early substance use warning signs such as mood changes, secretive behavior, or physical symptoms like drowsiness. Acting quickly—by reaching out to your treatment provider, restarting therapy, or joining a support group—can help prevent a brief lapse from becoming a full return to old patterns.5
Will my insurance cover opioid addiction treatment, and how do I verify coverage?
Insurance coverage for opioid addiction treatment varies, but most plans now include some support for key services—such as outpatient therapy, medication-assisted treatment, and often residential care—especially when opioid addiction symptoms are documented by a provider. To verify your benefits, gather your insurance cards and call the customer service number listed on the back. Ask specifically about coverage for substance use disorder treatment, including any requirements for pre-authorization or limits on visits and co-pays.5
How can I protect myself emotionally while supporting a loved one through addiction?
Supporting a loved one through opioid addiction symptoms can be emotionally exhausting, so protecting your own well-being is essential. Consider setting healthy boundaries—decide what you can and cannot do, and remind yourself that you are not responsible for your loved one’s choices or recovery. The Mayo Clinic highlights that families facing substance use warning signs often benefit from counseling to process stress and avoid burnout1.
What are the warning signs that my loved one is experiencing an overdose emergency?
Recognizing an opioid overdose emergency is critical and can save your loved one’s life. Warning signs include unresponsiveness or inability to wake, very slow or stopped breathing, blue or gray lips and fingertips, and a gurgling or snoring sound often called the "death rattle." Other symptoms may be pinpoint pupils and clammy or discolored skin. If you notice these opioid addiction symptoms or see someone losing consciousness after opioid use, act immediately: call 911, administer naloxone if available, and stay with them until help arrives.5
How does trauma-informed care differ from standard addiction treatment?
Trauma-informed care is a treatment approach that recognizes how past trauma—such as abuse, loss, or major life stress—can shape both opioid addiction symptoms and the recovery process. Unlike standard addiction treatment, which may focus mainly on stopping substance use, trauma-informed care creates a safe, supportive environment where a person’s experiences are honored and understood. Research shows that when treatment also considers underlying trauma, outcomes improve for those with substance use disorders and co-occurring mental health concerns.10
What should I do if I suspect my loved one is using fentanyl without knowing it?
If you suspect your loved one may be using fentanyl—knowingly or not—take action right away, as fentanyl is 50 to 100 times more potent than morphine and can cause a fatal overdose with even a tiny amount. Start by looking for new or severe opioid addiction symptoms, such as sudden drowsiness, slowed or stopped breathing, or blue-tinged lips. If you see any of these overdose warning signs, call 911 immediately and stay with your loved one until help arrives.4,6
How do I approach someone about their opioid use without pushing them away?
Approaching someone about their opioid use can feel daunting. The most effective way to begin is by expressing care and focusing on what you’ve noticed—such as changes in mood, routines, or physical health—rather than making accusations. The Mayo Clinic suggests statements like, “I’ve noticed you seem more withdrawn and tired lately, and I’m worried about you,” which can help reduce defensiveness and open up honest conversation.1
Can someone recover from opioid addiction while continuing to work full-time?
Yes, it is possible for someone to recover from opioid addiction symptoms while continuing to work full-time, especially with the right treatment plan and support. Outpatient programs are designed to offer flexible scheduling, allowing individuals to attend therapy sessions and receive medication-assisted treatment outside of work hours. This approach works best when symptoms are moderate, daily routines are largely maintained, and there is a strong support system at home.5
What is the typical cost range for outpatient opioid addiction treatment?
The typical cost range for outpatient opioid addiction treatment can vary widely depending on the services provided, insurance coverage, and individual treatment needs. While exact costs are not published in national research, most outpatient programs include counseling, medication management, and support sessions designed to address opioid addiction symptoms. Many insurance plans cover outpatient therapy and medication-assisted treatment, but a call to your provider is the best way to clarify what’s included.5
How long does opioid withdrawal last, and is it dangerous?
Opioid withdrawal usually begins within 6 to 24 hours after the last dose, with symptoms peaking around 72 hours and typically improving within 5 to 10 days. Common withdrawal symptoms include muscle aches, runny nose, sweating, nausea, diarrhea, dilated pupils, and trouble sleeping—these are physical signs you might notice if your loved one is struggling with opioid addiction symptoms. Although opioid withdrawal is rarely life-threatening on its own, it can feel extremely uncomfortable.7
Should I be worried if my loved one has both depression and opioid use issues?
Yes, it is cause for concern when a loved one is coping with both depression and opioid use issues, since these conditions often interact and make recovery more complicated. When depression and opioid addiction symptoms appear together, each can intensify the other. According to the National Institute of Mental Health, people with mental health disorders like depression are at higher risk for developing substance use problems, and effective recovery depends on addressing both conditions at once.10
What role can family members play in someone's recovery process?
Family members play a crucial role in a loved one's recovery from opioid addiction symptoms by offering emotional support, participating in treatment, and helping to create a stable, hopeful environment. Research shows that when families join therapy sessions, attend educational workshops, or take part in support groups, there is a 5.7% reduction in substance use frequency—equivalent to about three fewer weeks of drug use each year.9
Is medication-assisted treatment really recovery, or is it just replacing one drug with another?
Medication-assisted treatment (MAT) is widely recognized as a legitimate path to recovery—not just a substitution for opioid use. MAT uses FDA-approved medications like buprenorphine or methadone alongside counseling to stabilize brain chemistry, reduce cravings, and help individuals regain control over their lives. Research shows that MAT helps people with opioid addiction symptoms stay in treatment longer, lowers overdose risk, and improves recovery outcomes.5
References
- How to Tell if a Loved One is Abusing Opioids - Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/prescription-drug-abuse/in-depth/how-to-tell-if-a-loved-one-is-abusing-opioids/art-20386038
- Understanding the Opioid Overdose Epidemic - CDC. https://www.cdc.gov/overdose-prevention/about/understanding-the-opioid-overdose-epidemic.html
- SAMHSA National Helpline for Mental Health, Drug, and Alcohol Issues. https://www.samhsa.gov/find-help/helplines/national-helpline
- Fentanyl - National Institute on Drug Abuse (NIDA). https://nida.nih.gov/research-topics/fentanyl
- Opioid Use Disorder - Yale Medicine Fact Sheet. https://www.yalemedicine.org/conditions/opioid-use-disorder
- Recognizing Opioid Overdose - National Harm Reduction Coalition. https://harmreduction.org/issues/overdose-prevention/overview/overdose-basics/recognizing-opioid-overdose/
- Opioid Withdrawal - StatPearls - NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK526012/
- Xylazine - National Institute on Drug Abuse. https://nida.nih.gov/research-topics/xylazine
- Family Involvement in Treatment and Recovery for Substance Use Disorders - PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8380649/
- Finding Help for Co-Occurring Substance Use and Mental Disorders - NIMH. https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health





