How Does Outpatient Recovery Work?

Understanding Outpatient Recovery Models
Choosing to seek help is a brave first step, and for many, outpatient recovery offers the perfect balance between professional treatment and real-world responsibility. Unlike residential programs where you live at a facility, outpatient models allow you to sleep in your own bed and maintain your job or family duties while receiving structured clinical care.
It is important to understand that "outpatient" isn't a single type of treatment; it is a spectrum of care intensity designed to meet you exactly where you are. Whether you are stepping down from a hospital stay or seeking help for the first time, there is a model that fits your schedule and medical needs.
Comparison of Outpatient Care Levels
To help you decide which path is right for you, we have broken down the three primary tiers of outpatient services. Our team uses the ASAM Criteria (American Society of Addiction Medicine) to help place you in the safest and most effective tier.
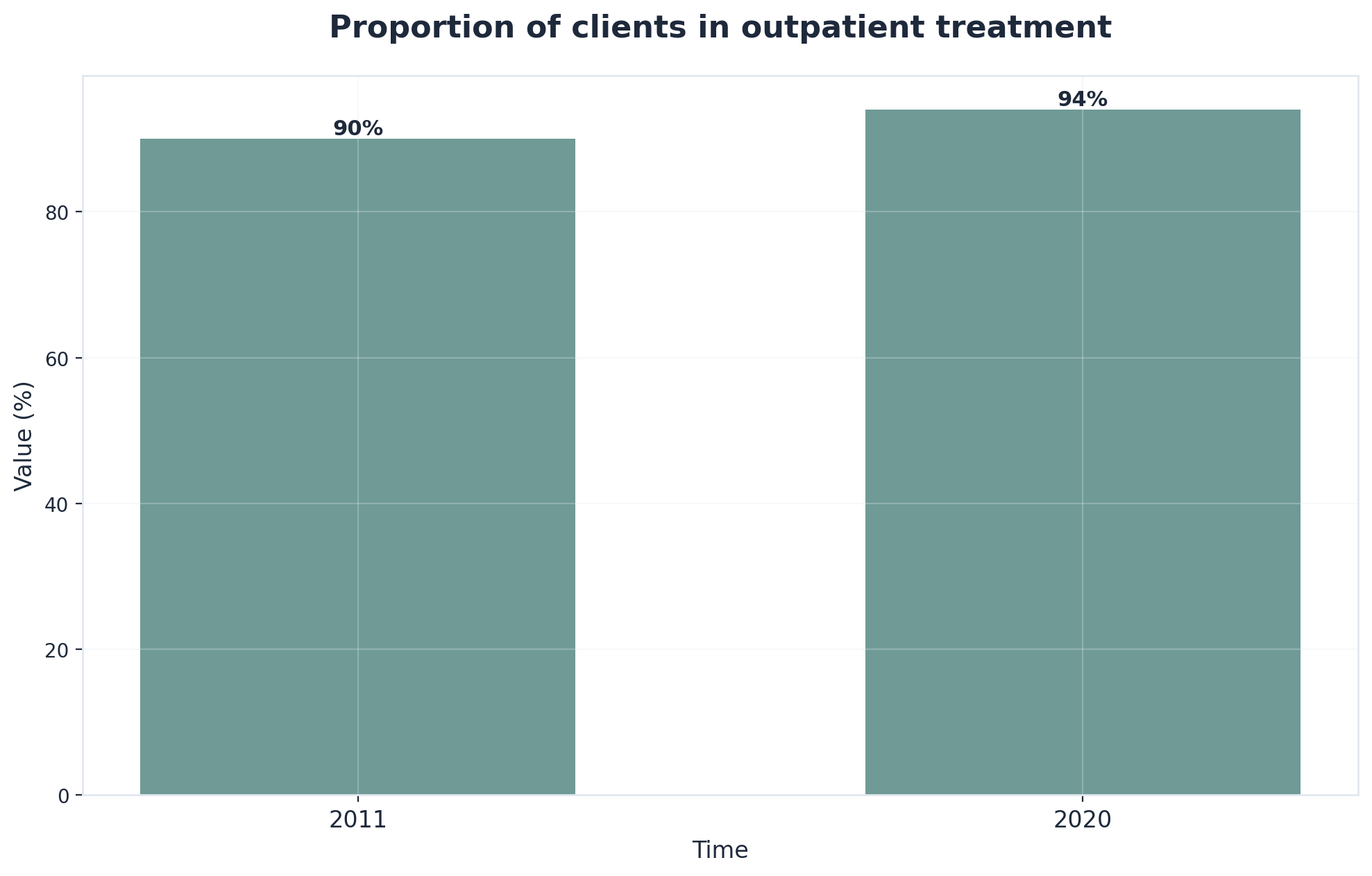
Did you know? National trends show that outpatient recovery is increasingly popular because it is accessible and effective. In fact, over 90% of addiction treatment is now delivered through outpatient models.10
Core Differences from Residential Care
The primary difference lies in your living situation. Residential care provides 24-hour supervision, which is critical for those in acute withdrawal or unsafe home environments. Outpatient care puts the keys in your hand—you practice your recovery skills in the "real world" every day. This allows you to integrate therapy immediately into your interactions with family and coworkers, but it also requires a higher degree of self-motivation.
Self-Assessment: Is Outpatient Recovery Right for You?
Honest reflection is the most important tool you have right now. While our clinicians will provide a professional assessment, you can start evaluating your readiness today. Outpatient care relies on your ability to navigate triggers outside of treatment hours.
"Recovery is not just about stopping substance use; it's about building a life where you don't need to use. Outpatient care helps you build that life in real-time."
Readiness Checklist
Review the following criteria. If you answer "Yes" to most of these, outpatient recovery is likely a viable option for you:
- Safe Environment: Do you have a home free of alcohol and drugs?
- Support System: Is there at least one person (family/friend) who supports your sobriety?
- Medical Stability: Are you past the phase of acute medical withdrawal (detox)?
- Motivation: Are you willing to attend all scheduled sessions and complete "homework" assignments?
- Transportation: Do you have a reliable way to get to the facility or access telehealth?
Clinical Placement Using ASAM Criteria
Professionals use the ASAM Criteria to determine your level of care. This isn't a guess; it's a multidimensional assessment that looks at six specific areas of your life7:
- Acute Intoxication/Withdrawal Potential: Do you need medical detox?
- Biomedical Conditions: Do you have physical health issues?
- Emotional/Behavioral Conditions: Do you have anxiety, depression, or trauma?
- Readiness to Change: How motivated are you?
- Relapse Potential: Can you manage cravings?
- Recovery Environment: Is your home safe?
Our team specializes in this assessment. If you are unsure where you fit, we can conduct this evaluation to ensure you aren't taking on too much, too soon.
Outpatient Recovery Treatment Components
Effective treatment is more than just "talk therapy." Our outpatient services utilize a comprehensive framework of evidence-based practices designed to rewire the brain and change behavior patterns.
Evidence-Based Therapies
We integrate specific therapeutic modalities that have been proven to treat addiction and co-occurring disorders.
Cognitive-Behavioral Therapy (CBT)
CBT helps you identify the specific thoughts ("I can't handle this stress") that lead to behaviors (using substances). By changing the thought, you change the outcome. Studies show CBT results in high success rates for maintaining sobriety.2
Dialectical Behavior Therapy (DBT)
Originally designed for emotional regulation, DBT is excellent for those with trauma or intense mood swings. It teaches mindfulness, distress tolerance, and emotional regulation skills.
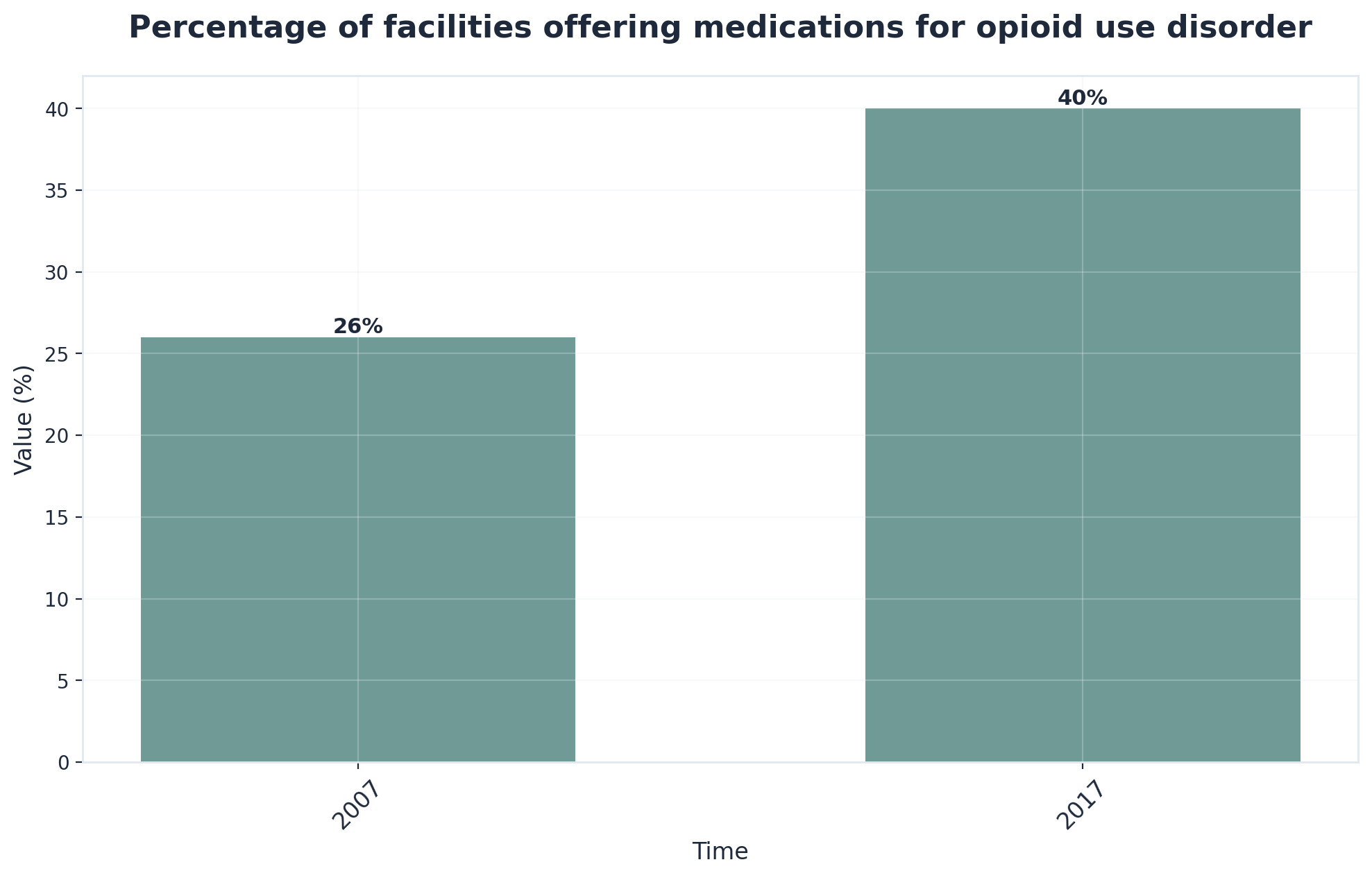
Medication-Assisted Treatment (MAT)
MAT combines behavioral therapy with medications (like buprenorphine or naltrexone). It is the "gold standard" for opioid and alcohol use disorders, reducing overdose risk by over 50%.5
Building Your Recovery Framework
Success in outpatient recovery requires a plan. We work with you to create a Personalized Treatment Plan that includes:8
- Goal Setting: Specific, measurable milestones (e.g., "Attend 90 meetings in 90 days").
- Care Coordination: We communicate with your primary care doctor and family (with permission) to ensure everyone is on the same page.
- Aftercare Planning: We start planning your exit strategy on day one to ensure you have support when formal treatment ends.

Your Next 30 Days: Action Plan
Looking at the big picture can be overwhelming. Let's break down your first month of outpatient recovery into actionable steps.
- Week 1: Stabilization & Logistics
Focus on the basics. Complete your intake assessment and verify your insurance benefits. Clear your home of any substances. Tell your "safe people" that you are starting treatment so they can support you. - Weeks 2-3: Routine & Skill Building
Attend every scheduled session—consistency is key. Start using a journal to track triggers. If you are in IOP, you will likely be attending groups 3-4 times a week. Begin practicing "saying no" in low-stakes situations. - Week 4: Review & Adjust
Sit down with your counselor to review your treatment plan. What is working? What feels too difficult? We will adjust your care level if needed. Celebrate your first month of progress!
Ready to start Week 1? Our admissions team is available to help you verify insurance and schedule your assessment.
Begin Your Recovery Journey in South Portland
Taking the first step toward recovery requires courage, and finding appropriate support can make all the difference. Individuals struggling with addiction deserve access to compassionate, evidence-based treatment designed to address their unique needs—care that recognizes both the medical complexities of chemical dependency and the personal journey each person brings.
Recovery is possible, and help is available. If you or someone you care about is ready to explore treatment options, taking action today can change everything. Call for a confidential assessment to discuss your specific situation, learn about available treatment approaches, and speak with an admissions counselor who can help create a personalized plan that supports healing and growth.
You don't have to have all the answers. You just need to recognize the need for change. Connect with us today for free benefits verification and a personalized path forward.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
.webp)
Frequently Asked Questions
It is normal to have questions about costs, timing, and privacy. Here are the most common questions we hear from clients considering outpatient care.
What does outpatient treatment cost, and will my insurance cover it?
The cost of outpatient recovery treatment varies based on care level and insurance. While out-of-pocket costs for private pay can range from $1,000 to $10,000+ depending on the program length, most insurance plans (private, Medicaid, government) cover these services. You typically pay only deductibles or copays (often $20-$75 per session). Our team handles benefits checks to clarify your specific coverage.
Can I continue working full-time while attending outpatient treatment?
Yes. Over 90% of people in addiction treatment choose outpatient care specifically for this flexibility. Programs offer evening and early morning sessions designed to fit around work schedules, allowing you to maintain employment while receiving clinical support.10
How do I know if I need intensive outpatient or standard outpatient care?
The decision relies on the ASAM Criteria. Intensive Outpatient (IOP) is best if you need structure (9-20 hours/week) and have a higher risk of relapse. Standard outpatient (1-9 hours/week) is for those with stable home environments and strong support systems who need maintenance therapy.7
What happens if I also have anxiety or depression along with substance use?
This is known as a co-occurring disorder. Our outpatient programs treat both simultaneously using integrated therapies like CBT and DBT. Addressing mental health alongside addiction is standard practice and significantly improves long-term recovery outcomes.4
Is medication-assisted treatment really effective?
Yes. MAT is not replacing one addiction with another; it is a medical intervention. Research shows MAT can reduce opioid overdose deaths by at least 50%. It stabilizes brain chemistry to block cravings, allowing you to focus on therapy and lifestyle changes.5
How long does outpatient treatment typically last?
Programs typically run 8 to 16 weeks, but duration is personalized. You might start with 30 days of intensive care and step down to weekly sessions for several months. Research supports longer engagement for better outcomes.10
What if I've tried outpatient treatment before and relapsed?
Relapse is often a sign that the treatment plan needs adjusting, not that you failed. We can modify the level of care, introduce medication support, or increase family involvement. Re-engaging with support immediately is the most effective response to relapse.6
Can my family be involved in my outpatient treatment?
Absolutely. Family involvement is strongly linked to better recovery outcomes. We offer family counseling and educational workshops to help loved ones understand addiction, set boundaries, and become active partners in your recovery.8
What's the difference between outpatient treatment and AA/NA?
Outpatient treatment is clinical care led by licensed medical professionals (therapists, doctors) providing evidence-based therapies and medication. AA/NA are peer-led support groups. The most effective approach often combines both clinical treatment and peer support.
Will my employer find out I'm in treatment?
No. HIPAA laws protect your privacy; we cannot share information with employers without your written consent. Flexible scheduling also helps you attend appointments without raising workplace questions.
How do I transition from residential treatment to outpatient care?
A 'step-down' plan is essential. We coordinate with your residential facility to ensure no gap in care. This involves scheduling your first outpatient appointment before you leave residential care and setting up a support network immediately.
What if I have past trauma?
Trauma-informed care is central to our approach. We use therapies like DBT and EMDR (where available) to process trauma safely without overwhelming you, recognizing that trauma is often a root cause of substance use.
Can I attend outpatient treatment if I'm still using substances?
Yes. You do not need to be 'perfect' to start. We meet you where you are. We can help with harm reduction, motivation, and medical stabilization to help you stop using safely.
What support is available after I complete outpatient treatment?
Recovery is ongoing. We provide aftercare planning which may include alumni groups, less frequent check-in therapy sessions, and connections to community resources to ensure you remain supported long-term.
References
- Medications for Opioid Use Disorder. https://nida.nih.gov/research-topics/medications-opioid-use-disorder
- Cognitive-Behavioral Therapy for Substance Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC2897895/
- Effects of Medication-Assisted Treatment (MAT) for Opioid Use. https://pmc.ncbi.nlm.nih.gov/articles/PMC7302321/
- Dual Diagnosis (Co-Occurring Disorders). https://my.clevelandclinic.org/health/diseases/24426-dual-diagnosis
- A Ray of Hope: The Effectiveness of Medication-Assisted Treatment for Opioid Addiction. https://www.cpdaac.org/post/a-ray-of-hope-the-effectiveness-of-medication-assisted-treatment-mat-for-opioid-addiction
- Relapse Prevention and the Five Rules of Recovery. https://pmc.ncbi.nlm.nih.gov/articles/PMC4553654/
- About The ASAM Criteria. https://www.asam.org/asam-criteria/about-the-asam-criteria
- Family Involvement in Treatment and Recovery for Substance Use. https://pmc.ncbi.nlm.nih.gov/articles/PMC8380649/
- Using Motivational Interviewing in Substance Use Disorder Treatment. https://library.samhsa.gov/sites/default/files/PEP20-02-02-014.pdf
- Intensive Outpatient Treatment and the Continuum of Care. https://www.ncbi.nlm.nih.gov/books/NBK64088/





