Xylazine Addiction and Recovery: A Guide

Understanding Xylazine's Role in Overdoses and Xylazine Addiction Treatment Maine
What Xylazine Is and Why It's Dangerous
In this section, you'll learn what xylazine is, why it has become a unique threat within the drug supply, and how its pharmacology increases the risk of overdose and harm. You’ll know you’ve understood this topic when you can explain why standard opioid overdose responses are often ineffective when xylazine is present and recognize the specific medical dangers associated with xylazine addiction treatment Maine protocols.
Xylazine is a non-opioid veterinary tranquilizer originally developed for animal sedation and not approved for human use. Increasingly, it is found mixed with illicit opioids such as fentanyl, making detection and response more complicated for professionals. Unlike opioids, which primarily affect the brain’s mu-opioid receptors, xylazine acts on alpha-2 adrenergic and kappa opioid receptors.
"Because of this, naloxone—the go-to opioid overdose reversal medication—cannot reverse xylazine’s effects, often leaving emergency responders with limited options beyond rescue breathing and advanced medical care." 1
Xylazine’s danger extends beyond overdose risk. It is strongly linked to severe, necrotic skin wounds that can develop at injection sites or even on other parts of the body, increasing the risk of infection and long-term tissue damage. These wounds often require specialized wound care and can complicate recovery. The addition of xylazine to the illicit drug supply has introduced new clinical challenges for addiction professionals, particularly in developing effective xylazine addiction treatment Maine and elsewhere.4
Practice This: Create a fact sheet that explains, in plain language, why xylazine is uniquely hazardous compared to traditional opioids. You’re ready for the next level when you can describe the specific reasons why xylazine-adulterated drugs increase overdose risk and complicate care.
Next, explore how national and regional data highlight the impact of xylazine’s spread.
National Trends and Regional Impact Data
In this section, you'll learn how xylazine's spread has reshaped overdose patterns in the United States and how these shifts are reflected in both national and Maine-specific data. You'll know you've mastered this when you can interpret key statistics and identify how trends inform the need for xylazine addiction treatment Maine and other regions.
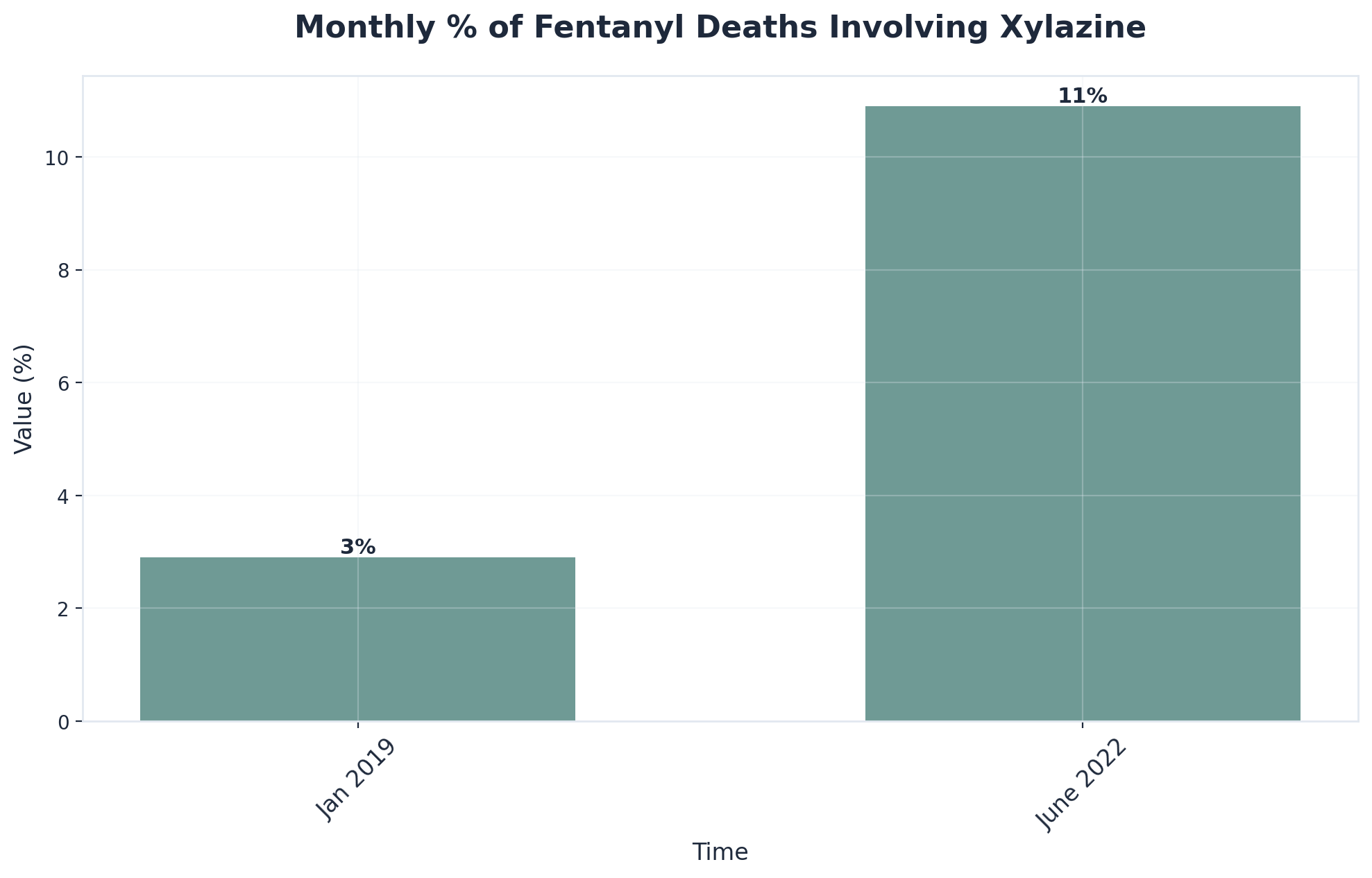
Nationally, xylazine’s presence in the illicit drug supply has increased sharply. The percentage of fentanyl-related overdose deaths involving xylazine jumped from 2.9% in January 2019 to 10.9% by June 2022, according to the CDC’s surveillance data. Some states have seen even more dramatic rises.1
Regionally, the South and West experienced the fastest growth in xylazine detections. These data point to a rapid and uneven spread, requiring adaptable, regionally informed responses. For professionals focused on xylazine addiction treatment Maine, this means staying current with both local and national epidemiological trends.
Practice This: Analyze overdose surveillance data from your local health department. Map out recent changes in xylazine involvement and discuss implications for clinical decision-making.
You’re ready for the next level when you can explain how emerging data should shape regional outreach and intervention strategies. Next, examine the specific medical and psychological consequences of xylazine use, including severe skin and tissue injuries.
Physical and Psychological Effects in Xylazine Addiction Treatment Maine
Severe Skin Wounds and Medical Complications
In this section, you'll learn to identify the hallmark physical complications of xylazine use, focusing on why skin wounds are so common and difficult to manage. You'll know you've mastered this topic when you can describe the appearance, risks, and clinical care challenges of xylazine-related ulcers—skills essential for planning effective recovery support in xylazine addiction treatment Maine.
Xylazine is notorious for causing deep, necrotic skin ulcers that are distinct from typical injection-related infections. These wounds can develop not just at injection sites, but also on other areas of the body, sometimes even where xylazine wasn't directly injected.
Analogy: Imagine a corrosive substance that damages tissue from the inside out, rather than a simple surface cut. Unlike standard abscesses, xylazine-induced ulcers are slow to heal, highly susceptible to infection, and often require multi-disciplinary wound care.
In Puerto Rico, for example, researchers found that 38.5% of people using xylazine developed skin ulcers, compared to just 6.8% of those who did not use the drug.4
Practice This: Create a visual guide or checklist for clinical staff, outlining how to distinguish xylazine-related wounds from other types of skin injuries. Include indicators such as depth, necrosis, and location.
You’re ready for the next level when you can communicate wound risks and care needs clearly to both medical teams and patients. Next, explore the withdrawal symptoms and systemic health risks associated with xylazine dependence.
Withdrawal Symptoms and Health Risks
In this section, you'll explore the core withdrawal symptoms and systemic health risks linked to xylazine dependence—knowledge that is essential for developing safe, effective xylazine addiction treatment Maine. Mastery of this topic means being able to recognize not just the discomfort of withdrawal, but the broader health threats that can emerge during detox and beyond.
Xylazine withdrawal sets itself apart from opioid withdrawal in both intensity and complexity. Individuals may experience severe anxiety, agitation, tremors, rapid heart rate, high blood pressure, and pronounced insomnia. Some withdrawal symptoms can persist for weeks, unlike the more predictable course of opioid withdrawal.
Comparison: Opioid vs. Xylazine
Because xylazine acts on alpha-2 adrenergic and kappa opioid receptors, abrupt cessation can trigger autonomic instability and profound psychological distress—think of the body’s "brakes" and "accelerator" malfunctioning at the same time, leading to unpredictable swings in mood, blood pressure, and heart rate.4
On the health risk front, xylazine use is associated with impaired healing, increased risk of infection, and cardiovascular complications. Respiratory depression remains a primary danger during intoxication and early withdrawal, especially when xylazine is mixed with opioids. These risks demand coordinated medical and behavioral oversight throughout recovery.1
Practice This: Draft a withdrawal monitoring checklist that includes both physical and psychological symptoms unique to xylazine. Share it with your care team and discuss protocols for escalation.
You’re ready for the next level when you can confidently differentiate xylazine withdrawal from opioid withdrawal and plan for complex health monitoring. Next, review which evidence-based treatment models are most effective for outpatient xylazine addiction recovery.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Evidence-Based Treatment Approaches
Medication-Assisted Treatment Protocols
In this section, you'll learn how medication-assisted treatment (MAT) protocols are being adapted for xylazine addiction treatment Maine, and how to evaluate their effectiveness in outpatient and professional settings. You will know you’ve mastered this material when you can describe the unique pharmacological considerations for xylazine, draft an MAT plan that integrates both opioid and non-opioid strategies, and explain the limitations and opportunities for MAT in this context.
MAT for xylazine addiction presents a distinct challenge: while medications like buprenorphine or methadone can address opioid dependence, there is currently no approved pharmacological agent that directly counters xylazine’s effects. This is because xylazine acts primarily on alpha-2 adrenergic and kappa opioid receptors, pathways not targeted by standard opioid use disorder medications.1
As a result, MAT protocols often require careful layering. A typical clinical logic flow might look like this:
For those pursuing the Business Application track, integrating MAT into organizational workflows means developing rapid screening tools to identify xylazine exposure and collaborating with prescribers to individualize protocols. For Personal Use, understanding the need for comprehensive support—including medication for sleep or anxiety—can empower clients to advocate for themselves during treatment planning.
Practice This: Create a draft MAT protocol for a hypothetical outpatient client with combined opioid and xylazine exposure. Include medication selection, symptom monitoring, and escalation criteria for medical complications.
You’re ready for the next level when you can explain why MAT for xylazine must go beyond standard opioid protocols and when you can coordinate care across medical and behavioral teams. Next, compare how therapeutic and psychosocial interventions complement MAT in effective xylazine addiction recovery.
Therapeutic Interventions and Support
In this section, you'll learn how evidence-based therapeutic interventions and structured psychosocial support are integral to xylazine addiction treatment Maine. You’ll know you’ve gained proficiency when you can design a layered care plan that blends clinical therapies with community support, and when you can adapt approaches for both organizational and individual needs.
The complexity of xylazine addiction requires more than medication alone. Best-practice models emphasize a combination of:4
- Cognitive Behavioral Therapy (CBT): Works like a mental toolkit—helping clients identify and reframe thought patterns that fuel substance use.
- Dialectical Behavior Therapy (DBT): Adds tools for emotional regulation and distress tolerance, essential for managing the intense mood swings and anxiety that often accompany xylazine withdrawal.
- Motivational Interviewing: Leverages a non-confrontational approach, guiding individuals to clarify their own reasons for change.
- Trauma-Informed Care: Recognizes that past trauma often intersects with substance use, and adapts therapy to avoid re-traumatization.
On the Business Application track, building a multidisciplinary team—including therapists, case managers, and peer support—can streamline care and improve outcomes. For Personal Use, engaging in group therapy or alumni networks offers accountability and connection, reducing isolation during recovery. Continuous psychoeducation on wound care, relapse prevention, and life skills rounds out the recovery process.
Practice This: Map out a weekly schedule that integrates individual therapy, skills groups, and peer support for a hypothetical outpatient client with xylazine dependence.
You’re ready for the next level when you can coordinate these interventions into a seamless, flexible plan that adapts to changing needs across the recovery timeline. Next, discover how recovery planning can be structured to support working professionals balancing treatment with career obligations.4
Recovery Planning for Working Professionals
Balancing professional responsibilities with recovery requires a structured approach that acknowledges the realities of workplace demands. Working professionals face unique challenges when seeking treatment, including concerns about job security, client relationships, and career momentum. A comprehensive recovery plan addresses these factors while prioritizing health and long-term stability.
Effective recovery planning begins with an honest assessment of current commitments and identifying which aspects of work life can be maintained during treatment. This includes evaluating workload capacity, communication strategies with employers or colleagues, and establishing boundaries that protect recovery time. Many professionals benefit from exploring flexible treatment options that accommodate work schedules rather than requiring extended absences.4
Intensive Outpatient Programs (IOP) and Partial Hospitalization Programs (PHP) offer structured support while allowing individuals to maintain employment. These programs provide evidence-based therapies such as Cognitive Behavioral Therapy, Dialectical Behavioral Therapy, and motivational interviewing during morning, afternoon, or evening sessions. This scheduling flexibility enables professionals to attend client meetings, manage projects, and fulfill responsibilities while receiving comprehensive care.
Workplace Coping Strategies (Click to Expand)
Recovery planning also involves developing practical coping strategies for workplace stressors that may trigger substance use. Professionals learn emotional regulation techniques, communication skills, and relapse prevention strategies that apply directly to high-pressure work environments. These tools become essential for navigating challenging situations, managing stress without substances, and maintaining professional performance throughout recovery.
For professionals requiring additional support, medication-assisted treatment offers a practical advantage during early recovery by stabilizing withdrawal symptoms and reducing cravings that could otherwise impair cognitive function and work performance. This approach enables individuals to maintain focus during presentations, manage complex decision-making, and engage effectively with colleagues while their brain chemistry rebalances.
Coastal Recovery Partners' care coordination services function as a business efficiency tool, handling tasks like coordinating with insurance providers to minimize paperwork disruption, scheduling medical appointments around quarterly deadlines, and managing prescription refills without requiring time away from work. This coordinated approach allows professionals to focus on both recovery and career responsibilities without administrative burden.
A well-designed recovery plan recognizes that professional success and personal wellness are interconnected. By addressing both clinical needs and practical workplace considerations, individuals can pursue recovery while protecting the careers they've worked hard to build.
Frequently Asked Questions
How does xylazine withdrawal differ from traditional opioid withdrawal?
Xylazine withdrawal differs significantly from traditional opioid withdrawal in both symptoms and management. While opioid withdrawal typically involves muscle aches, nausea, and anxiety, xylazine withdrawal can cause severe agitation, high blood pressure, tremors, and profound insomnia. These symptoms may last longer and are less predictable, partly because xylazine affects alpha-2 adrenergic and kappa opioid receptors, leading to autonomic instability—imagine a car’s brakes and accelerator failing at the same time, creating unpredictable swings in heart rate and mood. This complexity requires more intensive monitoring and tailored xylazine addiction treatment Maine protocols.4
Can xylazine-related skin wounds heal completely with proper treatment?
Xylazine-related skin wounds can heal with proper treatment, but the process is often lengthy and challenging. Unlike typical abscesses, xylazine wounds are deep, necrotic, and slow to recover due to poor blood flow and increased infection risk. Complete healing is possible, especially with early intervention, multidisciplinary wound care, and support for underlying substance use. However, some individuals may experience lasting scarring or, in severe cases, require surgical intervention. Consistent care and coordinated xylazine addiction treatment Maine can improve outcomes, but ongoing risk of reinjury remains if substance use continues.4
What should emergency responders know about xylazine in overdose situations?
Emergency responders should know that standard opioid overdose protocols, such as administering naloxone, may not reverse the effects of xylazine. Xylazine can cause severe respiratory depression, bradycardia, and hypotension, but because it is not an opioid, naloxone does not address these symptoms. Instead, responders should focus on airway management, rescue breathing, and rapid transport to advanced medical care. Monitoring for prolonged sedation and cardiac instability is essential. Awareness of these differences is crucial for all xylazine addiction treatment Maine scenarios, as traditional approaches may be inadequate in these cases.1,4
How do outpatient programs accommodate professionals dealing with xylazine exposure?
Outpatient programs support professionals facing xylazine exposure by offering flexible scheduling—such as early morning, evening, or virtual sessions—to minimize disruption to work and personal obligations. Care teams coordinate individualized treatment plans, which may include medication management, wound care, and access to trauma-informed therapy. Confidentiality and discretion are emphasized, allowing professionals to seek help without risking their careers. Evidence shows that programs designed with adaptable scheduling and comprehensive care components improve treatment engagement and completion rates among working adults, including those navigating xylazine addiction treatment Maine.4
What is medetomidine and how does it compare to xylazine in treatment complexity?
Medetomidine is a veterinary sedative closely related to xylazine but is estimated to be 100 to 200 times more potent, making it a growing concern as it enters the illicit drug supply. Compared to xylazine, medetomidine causes even deeper sedation, more severe respiratory depression, and greater risk of overdose. Treatment complexity increases because standard emergency and withdrawal protocols are even less effective, and supportive care becomes more intensive. Outpatient teams addressing xylazine addiction treatment Maine now need to watch for medetomidine exposure, as its effects can further complicate detox, wound care, and overall recovery planning.6
How long does coordinated care typically last for xylazine-involved substance use?
Most coordinated care plans for xylazine-involved substance use last at least six to twelve months, but the exact duration varies with medical complexity and the persistence of skin wounds or psychological symptoms. Xylazine addiction treatment Maine typically involves ongoing wound care, behavioral therapy, medication management, and frequent monitoring, especially since withdrawal and tissue healing can both be prolonged. National guidelines emphasize that longer-term engagement—often extending beyond a year—improves stability, reduces relapse risk, and supports full reintegration for professionals managing work and life obligations. Effective care is highly individualized, with duration adjusting to the client’s progress and evolving needs.4
Conclusion
Recovery and career success are not mutually exclusive—this is the reality that thousands of working professionals navigate daily. The integration of structured treatment into professional life requires neither career sacrifice nor compromised care. It demands treatment models that recognize the complexity of maintaining client relationships, meeting quarterly targets, and advancing professionally while addressing substance use with the seriousness it deserves.
Coastal Recovery Partners structures programs specifically for this reality. Treatment options accommodate the demands of professional life—quarterly deadlines, client relationships, and career advancement goals—through scheduling that works around existing commitments and clinical approaches that address both immediate recovery needs and long-term sustainability. The programs integrate evidence-based therapeutic methods with practical relapse prevention strategies, all delivered within a framework that respects the professional identities individuals have built.
The path forward doesn't require choosing between professional identity and health. It requires treatment structures that acknowledge both as essential, clinical support that addresses underlying factors without derailing momentum, and the recognition that sustainable recovery is built within the context of real life—not apart from it. Working professionals have already demonstrated the discipline, planning, and commitment required for recovery. The right treatment structure simply provides the clinical foundation to apply those strengths effectively.
Remember that recovery is a journey of rebuilding trust—in yourself, in others, and in the process of healing. If you are ready to explore your options, reach out to Coastal Recovery today. We're here to help guide you toward a future defined not by your past, but by your resilience and hope.
References
- National Institute on Drug Abuse. Xylazine. https://nida.nih.gov/research-topics/xylazine
- DEA. The Growing Threat of Xylazine and its Mixture with Illicit Drugs. https://www.dea.gov/sites/default/files/2022-12/The%20Growing%20Threat%20of%20Xylazine%20and%20its%20Mixture%20with%20Illicit%20Drugs.pdf
- NCBI. Xylazine Prevalence and Concentration in the Los Angeles Fentanyl Supply. https://pmc.ncbi.nlm.nih.gov/articles/PMC12132135/
- Johns Hopkins. Xylazine's Growing Impact on Drug Use and Treatment Options. https://publichealth.jhu.edu/2024/xylazines-growing-impact-on-drug-use-and-treatment-options
- CDC. Notes from the Field: Xylazine identified in Connecticut. https://www.cdc.gov/mmwr/volumes/70/wr/mm7037a5.htm
- Substance Use Philly. Medetomidine: What you need to know about the new street drug. https://www.substanceusephilly.com/medetomidine
- White House. Fentanyl Adulterated or Associated with Xylazine Emerging Threat Response Plan. https://bidenwhitehouse.archives.gov/wp-content/uploads/2023/07/FENTANYL-ADULTERATED-OR-ASSOCIATED-WITH-XYLAZINE-EMERGING-THREAT-RESPONSE-PLAN-Report-July-2023.pdf
- UNC Health. Scientists Discover Surprising Details about Xylazine in Combination with Fentanyl. https://news.unchealthcare.org/2024/05/scientists-discover-surprising-details-about-xylazine-in-combination-with-fentanyl/
- NCBI. Multidisciplinary Guidance to Care for Persons With Xylazine-Associated Wounds. https://pmc.ncbi.nlm.nih.gov/articles/PMC12125673/
- CDC. What You Should Know About Xylazine. https://www.cdc.gov/overdose-prevention/about/what-you-should-know-about-xylazine.html





