Benzo Rehab for Working Professionals: A Guide

Understanding Benzodiazepine Dependence
How Dependence Develops in Professionals
For professionals seeking benzo rehab Maine options, understanding the physiological progression of dependence is the first step toward reclaiming control. Dependence rarely happens overnight; it is a gradual process often initiated by a legitimate prescription for anxiety, insomnia, or work-related stress. In high-pressure roles, professionals may begin taking benzodiazepines as prescribed, but ongoing deadlines and performance anxiety can lead to increased reliance.
"Imagine dependence like a slow leak in a tire: at first, things seem stable, but over time, small changes add up until normal function is compromised."
Research indicates that physical dependence can develop after just three to four weeks of continuous use, even when following prescribed doses. The professional environment can subtly reinforce this cycle. When benzodiazepines provide quick relief, it becomes tempting to utilize them as a routine fix for work stress. Over time, tolerance builds, requiring higher or more frequent doses to achieve the same effect. Dependence may go unnoticed until withdrawal symptoms appear between doses, often mistaken for job burnout or chronic stress.2,10
Professional Assessment: Early Warning Signs
If you recognize these signs in your daily work life, it may indicate developing dependence:
- Inter-dose Withdrawal: Feeling anxious or irritable a few hours before your next scheduled dose.
- Preoccupation: Worrying about running out of medication during business trips or long meetings.
- Performance Masking: Taking medication specifically to handle presentations or difficult conversations.
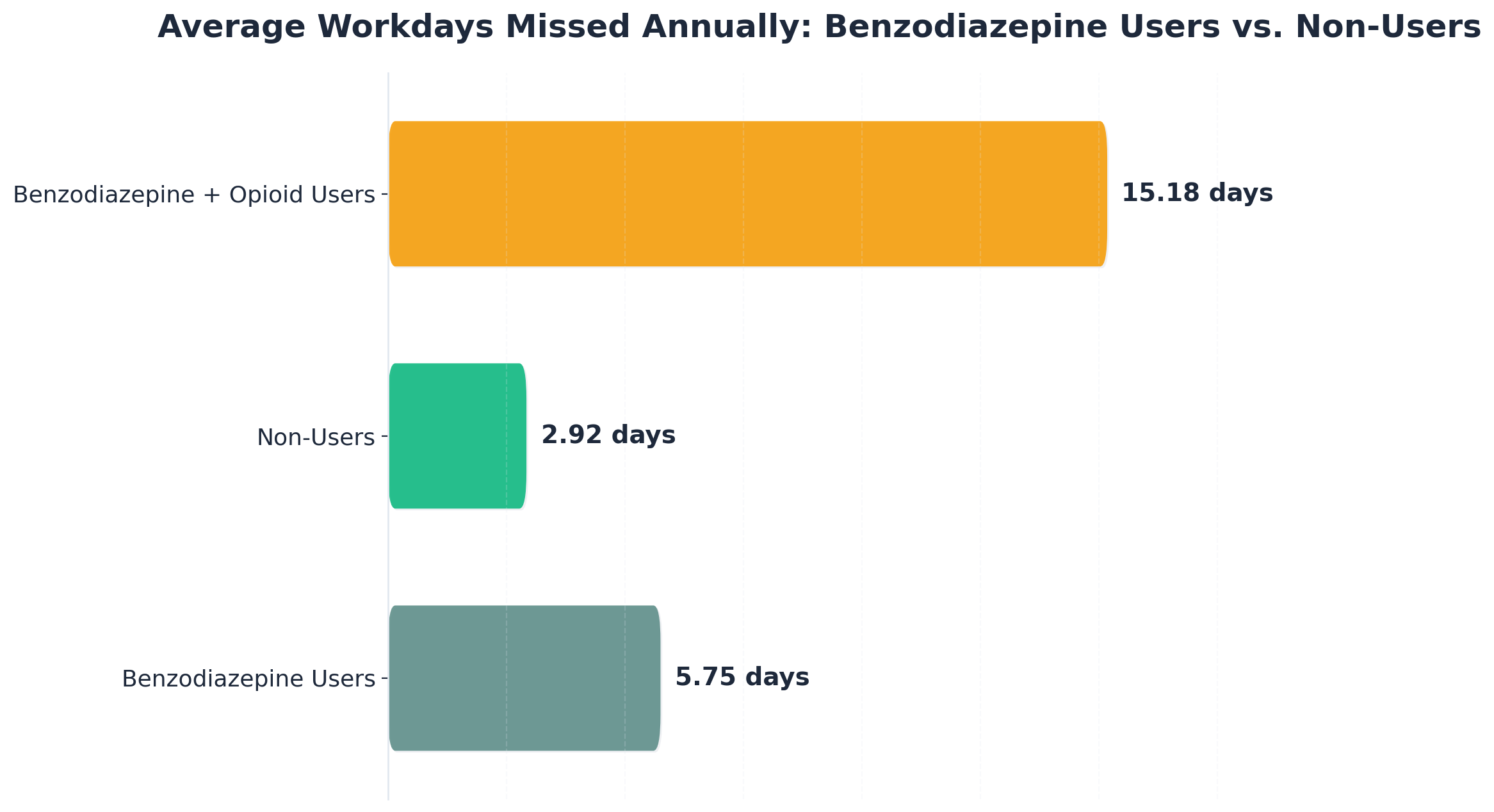
Workplace Impact and Productivity Loss
Benzodiazepine dependence often creates a hidden drain on workplace productivity. Imagine a high-performing team member whose efficiency slowly slips: deadlines are missed, mistakes increase, and meetings feel foggy. For professionals, this decline can be gradual and masked by efforts to compensate, such as working longer hours or avoiding collaboration.
Beyond attendance, cognitive effects can disrupt workflow. These symptoms often appear before noticeable absenteeism and may be mistaken for stress or fatigue. Team dynamics suffer as affected professionals may withdraw from group projects or struggle with communication. In leadership roles, this can ripple through entire teams, reducing morale and project outcomes.
Evidence-Based Tapering Protocols in Benzo Rehab Maine
Safe Dose Reduction Schedules
Benzodiazepine tapering is akin to slowly stepping down from a moving escalator: if you jump too quickly, you risk falling, but gradual steps keep you steady. In evidence-based benzo rehab Maine settings, dose reductions typically occur at a pace of 5% to 10% every two to four weeks, with adjustments based on individual response and clinical judgment.1
This slow, structured approach minimizes withdrawal symptoms such as anxiety, insomnia, and agitation, which can be disruptive for professionals balancing work and recovery obligations. The protocol generally follows these steps:
- Stabilization: Switching to a longer-acting benzodiazepine to ensure consistent blood levels.
- Initial Reduction: Small decreases to test physiological response.
- Plateau Periods: Pausing reductions during high-stress work periods to maintain stability.
- Final Taper: Micro-reductions to safely cease medication.
For professionals, a gradual taper allows continued workplace engagement and reduces productivity loss. Individuals can monitor their own symptoms and communicate openly with their care team about progress and setbacks.
Medical Supervision and Support Systems
Medical supervision is the safety net of any evidence-based benzodiazepine taper. Ongoing clinical oversight helps prevent withdrawal complications and allows for real-time adjustments. In practice, this means regular check-ins, symptom tracking, and prompt medication changes when side effects or setbacks occur. Having a coordinated care team—including physicians, therapists, and care coordinators—improves outcomes and keeps the process on track.7
Professionals often face unique stressors. Medical supervision ensures that dose reductions and mental health symptoms are monitored together, so treatment can quickly adapt to life events or workplace demands. Support systems such as group therapy, peer support, and care coordination also provide accountability and emotional reinforcement, which research links to improved retention and recovery rates.7
Flexible Treatment Models for Professionals in Benzo Rehab Maine
Outpatient Programs That Fit Work Schedules
Outpatient programs are often compared to executive education for professionals—structured, scheduled, and focused, but adaptable to existing commitments. Unlike residential rehab, outpatient models such as Intensive Outpatient Programs (IOPs) and Partial Hospitalization Programs (PHPs) offer morning, afternoon, or evening sessions, allowing professionals to attend therapy outside of core work hours.
This flexibility is especially valuable, as research highlights that maintaining employment during treatment is linked to better long-term recovery outcomes and improved quality of life. Flexible scheduling goes beyond session timing. Many benzo rehab Maine programs coordinate care around peak workplace demands, adjust frequency of therapy during major projects, and offer remote or hybrid participation for those who travel or work irregular shifts.7
Business Application: For organizations, supporting access to outpatient rehab can reduce absenteeism, sustain productivity, and demonstrate a commitment to employee well-being. Personal Use: Professionals can integrate treatment into their weekly routines without disclosing details to colleagues or taking extended leaves, reducing stigma and career disruption.
Integrated Dual Diagnosis Care
Effective recovery for professionals often requires more than just treating substance dependence—mental health conditions such as anxiety, depression, or trauma frequently occur alongside benzodiazepine use. Research shows that about 50% of people with a substance use disorder also have a co-occurring mental health disorder, highlighting the importance of integrated care.5

The Dual Diagnosis Approach
Imagine a two-sided coin: one side represents substance use, the other mental health. Ignoring one side means the coin can’t truly be whole. Integrated care addresses both simultaneously.
In practice, dual diagnosis programs combine evidence-based therapies like cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT) to address both sides of the coin simultaneously. This might include learning emotional regulation skills, practicing mindfulness, or exploring workplace stressors that fuel both anxiety and substance use. A trauma-informed approach is also essential, as past experiences can shape current behaviors and treatment responses.
Building Long-Term Recovery Skills
Therapeutic Approaches for Professionals
Professionals benefit most from treatment models that recognize the unique pressures of demanding careers. Therapies are often combined with mindfulness training, values-based exercises, and communication skills, tailored to real-world work scenarios. These practices help professionals anticipate triggers, manage anxiety, and maintain focus in challenging environments.
Cognitive Behavioral Therapy (CBT) Helps individuals identify and reframe workplace stressors and unhelpful thought patterns.
Dialectical Behavior Therapy (DBT) Emphasizes emotional regulation and distress tolerance—key skills for handling high-pressure situations. Research demonstrates that DBT can significantly improve treatment retention, with 64% of patients remaining in therapy compared to just 27% with standard approaches.
Relapse Prevention in High-Stress Careers
Relapse prevention in benzo rehab Maine is like maintaining a well-serviced car on a busy commute—routine check-ins, adaptive navigation, and strong support keep everything running smoothly, even when traffic gets tough. For professionals, key strategies include identifying high-risk situations at work (such as deadlines or conflicts), developing a toolbox of coping skills, and building a reliable accountability network.
Research highlights that coordinated support—including therapy, peer groups, and ongoing care—improves recovery retention and reduces relapse risk. Professionals can track stressors, set clear boundaries, and use regular self-assessments to spot and address early warning signs.7
Actionable Strategy: Draft a relapse prevention plan for a high-stress week, listing workplace triggers and specific coping responses.

Finding the Right Support in Maine
If you're reading this, you already know that recovery doesn't pause for professional responsibilities—and professional life doesn't wait for recovery to be complete. The challenge many face isn't whether to seek treatment, but how to access meaningful support without stepping away from the career, the team, or the identity they've worked years to build. This article explores how outpatient care in Maine can provide the structure and clinical support needed for sustainable recovery while keeping professional commitments intact.
Finding treatment that respects both recovery needs and work realities requires more than flexible hours—it requires a program designed around that balance from the ground up. Coastal Recovery Partners structures their outpatient approach specifically for this challenge, offering care at different intensity levels depending on where someone is in their recovery journey. Whether someone needs several sessions per week or is transitioning to less frequent support, the program adjusts to meet clinical needs without requiring extended absences from work. Sessions are available throughout the day, making it possible to attend treatment before work, during lunch hours, or in the evening.
The clinical approach combines therapies that address thought patterns and behaviors with strategies for managing triggers and building long-term coping skills. For those navigating both substance use and mental health concerns—something many professionals experience—treatment addresses both simultaneously rather than treating them as separate issues. When medication can support recovery, it's integrated with ongoing therapy and planning. Care coordination support helps navigate insurance questions and treatment decisions, reducing the administrative burden that often becomes its own obstacle. This integrated model recognizes that sustainable recovery happens when treatment fits into life, not when life stops for treatment.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Frequently Asked Questions
What happens if I need to switch between treatment program levels during recovery?
Switching between levels such as Intensive Outpatient (IOP), Partial Hospitalization (PHP), or standard Outpatient care is a common, flexible feature of benzo rehab Maine programs. Clinical teams regularly reassess your needs—if symptoms intensify, stepping up to a more structured program ensures stability; if progress is steady, transitioning to less intensive care supports independence while maintaining support. This adaptive approach is grounded in evidence that coordinated, ongoing care improves recovery outcomes and allows professionals to manage treatment alongside work obligations. Open communication with your treatment team makes these transitions smooth and responsive to both clinical and occupational demands.7
How do I manage withdrawal symptoms while maintaining my professional responsibilities?
Managing withdrawal symptoms while maintaining professional responsibilities involves coordinated, gradual strategies. In benzo rehab Maine, medically supervised tapers reduce withdrawal intensity by decreasing doses slowly—typically 5-10% every two to four weeks. This approach helps limit disruptions like anxiety, poor concentration, or sleep issues, which can otherwise impact work performance. Utilizing flexible outpatient programs allows professionals to attend therapy outside work hours, while evidence-based therapies (such as CBT or DBT) teach practical coping skills for stress and symptom management. Regular check-ins with a care team and honest communication about workplace needs are key to balancing recovery with ongoing job obligations.1,7
Can I continue taking my prescribed benzodiazepine during the initial treatment assessment?
Yes, you can generally continue taking your prescribed benzodiazepine during the initial assessment phase in benzo rehab Maine. Abruptly stopping benzodiazepines is not recommended due to the risk of severe withdrawal symptoms and potential medical complications. Instead, clinical teams use the assessment period to evaluate your current dose, usage patterns, and overall health before developing a gradual, individualized tapering plan. This patient-centered approach aligns with current guidelines, which emphasize slow dose reductions under medical supervision to ensure safety and maintain daily functioning during treatment. Open communication with your care team is encouraged throughout the process.1
What role does insurance play in covering outpatient benzodiazepine treatment programs?
Insurance plays a significant role in making outpatient benzodiazepine treatment programs accessible for professionals. Under the Mental Health Parity and Addiction Equity Act (MHPAEA), most employer-sponsored and individual health plans are required to cover substance use treatment—including benzo rehab Maine—on par with medical and surgical benefits. This means coverage for Intensive Outpatient Programs (IOPs), Partial Hospitalization Programs (PHPs), therapy sessions, and medication-assisted treatment must be comparable to other health benefits. However, coverage details—such as deductibles, co-pays, and preauthorization—can vary between plans. It is helpful to verify coverage specifics with your insurer or a treatment program’s care coordinator before starting care.9
How does treatment address both anxiety disorders and benzodiazepine dependence simultaneously?
Treatment for anxiety disorders and benzodiazepine dependence in benzo rehab Maine is integrated through dual diagnosis care. Professionals receive coordinated support that addresses both conditions at once—rather than treating anxiety or substance use in isolation. Evidence-based therapies like cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT) target anxious thinking, teach emotional regulation, and help develop coping skills for both work and personal stressors. Research shows about 50% of individuals with a substance use disorder also have a co-occurring mental health disorder, making this combined approach essential for lasting recovery. Clinical teams may also use medication management and trauma-informed care to further support both needs.5
What support systems are available after completing the primary treatment program?
After completing a primary treatment program in benzo rehab Maine, ongoing support systems help professionals sustain recovery and balance work commitments. Common options include structured aftercare groups, relapse prevention therapy, alumni networks, and ongoing access to outpatient counseling. Peer support—such as recovery groups or mentorship programs—provides connection and accountability, while periodic check-ins with care coordinators help monitor progress and address any setbacks. Research has shown that ongoing care coordination and support significantly improve long-term recovery outcomes for individuals with substance use disorders. These systems are designed to be flexible, allowing professionals to continue personal growth while maintaining career responsibilities.7
References
- Joint Clinical Practice Guideline on Benzodiazepine Tapering (2025). Source: ASAM/ACMT. URL not provided in source
- Management of benzodiazepine misuse and dependence. Source: PMC. URL not provided in source
- Trends in Nonfatal and Fatal Overdoses Involving Benzodiazepines. Source: CDC. URL not provided in source
- Productivity Loss Among Opioid and Benzodiazepine Users. Source: PMC. URL not provided in source
- Dual Diagnosis (Co-Occurring Disorders). Source: Cleveland Clinic. URL not provided in source
- Why Prescribed Benzo Patients Shouldn't Go To Detox or Rehab. Source: BenzoInfo.com. URL not provided in source
- Care Coordination Strategies for Patients Can Improve Substance Use Disorder Outcomes. Source: PEW Research. URL not provided in source
- Dialectical Behavior Therapy for Substance Abusers. Source: PMC. URL not provided in source
- The Mental Health Parity and Addiction Equity Act (MHPAEA). Source: CMS. URL not provided in source
- Work-Related Stressors and Increased Risk of Benzodiazepine Long-Term Use. Source: PMC. URL not provided in source





